Pulmonary arterial hypertension (PAH) is a devastating, rare, and progressive cardiovascular disorder characterized by the constriction of small pulmonary arteries and dangerously elevated blood pressure. This condition places immense strain on the heart, severely limits physical activity, and significantly reduces life expectancy, with a five-year mortality rate as high as 43%. New, effective treatments are urgently needed to improve patient outcomes and quality of life.
Recent findings from the phase 3 HYPERION trial (NCT04811092) offer significant hope, demonstrating that sotatercept (Winrevair; Merck & Co), when added to standard background therapy, dramatically reduces the risk of disease progression in adults recently diagnosed with PAH. These compelling results were presented at the 2025 European Respiratory Society Congress and simultaneously published in the prestigious New England Journal of Medicine.
Understanding Sotatercept and PAH
Sotatercept is a groundbreaking activin signaling inhibitor and the first of its kind approved for treating adults with PAH. Initially approved in 2024 to enhance exercise capacity, sotatercept works by modulating vascular proliferation. It rebalances pro-proliferative and anti-proliferative signaling pathways, inducing cellular changes that contribute to partial reversal of right ventricular remodeling, improved hemodynamics, and thinner vessel walls.
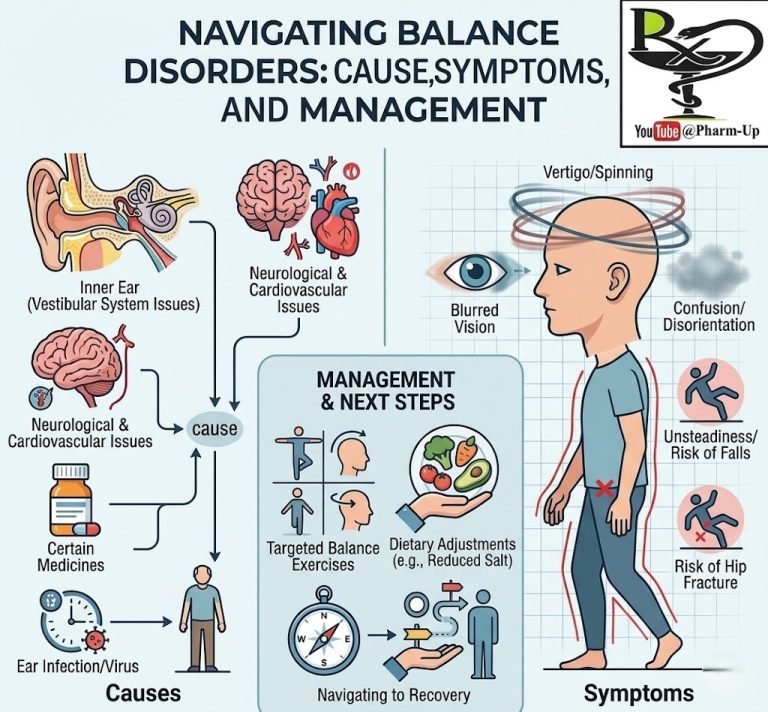
Pulmonary Arterial Hypertension (PAH) affects a limited number of individuals globally, leading to rapid disease progression, heart failure, and severely constrained physical activity. The underlying issue is the narrowing of the small arteries in the lungs, leading to increased blood pressure within these vessels.
HYPERION Trial: Early Intervention, Dramatic Results
The HYPERION trial specifically investigated the benefits of initiating sotatercept within the first year of a PAH diagnosis. The study enrolled 320 adults with FC II or III PAH who had been diagnosed less than one year prior and were already receiving double or triple background therapy, placing them at intermediate or high risk of disease progression. Participants were randomly assigned to receive either add-on subcutaneous sotatercept (escalating to a target dose of 0.7 mg/kg every three weeks) or a placebo.
After a median follow-up of 13.2 months, the results were striking:
- 76% Reduction in Clinical Worsening: Sotatercept reduced the risk of clinical worsening events by a remarkable 76% (hazard ratio [HR]: 0.24 [95% CI, 0.14—0.41]; P < .0001).
- Composite End Point: Clinical worsening was defined by a composite end point that included all-cause death, unplanned PAH-related hospitalization, atrial septostomy, lung transplantation, or PAH deterioration.
- Significant Event Rate Difference: Primary end point events occurred in only 17 patients (10.6%) in the sotatercept group, compared to 59 patients (36.9%) in the placebo group.
- Early and Sustained Benefit: Kaplan-Meier curves showed an early and sustained separation between the groups, with a treatment benefit observed within just six weeks of randomization.
- Consistent Efficacy Across Subgroups: The positive effects of sotatercept were consistent across all prespecified subgroups, including patients with idiopathic PAH, those with connective tissue disease, and patients on various background therapies.
Key Safety and Secondary Efficacy Indications
Beyond the primary end point, several key secondary end points reinforced sotatercept’s efficacy and favorable safety profile:
- Improved Exercise Performance: Only 8 patients (5.0%) on sotatercept experienced deterioration in exercise performance due to PAH, compared to 46 patients (28.8%) on placebo.
- Reduced Hospitalization: Unplanned hospitalization for worsening PAH occurred in 3 sotatercept-treated patients (1.9%) versus 14 placebo patients (8.8%).
- Mortality Rates: Death from any cause was observed in 7 sotatercept patients (4.4%) and 6 placebo patients (3.8%).
- Safety Profile: The overall safety profile was consistent with previous research. Adverse events (AEs) occurred at similar rates in both groups (89.4% for sotatercept vs. 90.0% for placebo), but serious AEs were more frequent in the placebo group.
- Common AEs: The most common AEs in the sotatercept group were epistaxis (nosebleeds, 31.9%) and telangiectasia (spider veins, 26.2%). Notably, no instances of atrial septostomy or lung transplantation were observed in the sotatercept group.
Dr. Vallerie McLaughlin, Director of the Pulmonary Hypertension Program at the University of Michigan, emphasized that the HYPERION trial’s patient population—early in their treatment journey, with co-morbidities, and older—accurately reflects real-world diagnoses. She expressed strong encouragement for sotatercept’s ability to significantly reduce clinical worsening events when initiated within the first year of diagnosis.
Implications for Pharmacists
For pharmacists, sotatercept represents a pivotal advancement in the management of PAH. By targeting the fundamental underlying factors of the disease, such as impaired blood flow and reduced exercise capacity, it offers a robust new avenue to significantly improve patient outcomes and enhance their quality of life. Pharmacists will play a critical role in patient education, ensuring adherence, and monitoring for adverse effects, thereby maximizing the therapeutic benefits of this innovative therapy.