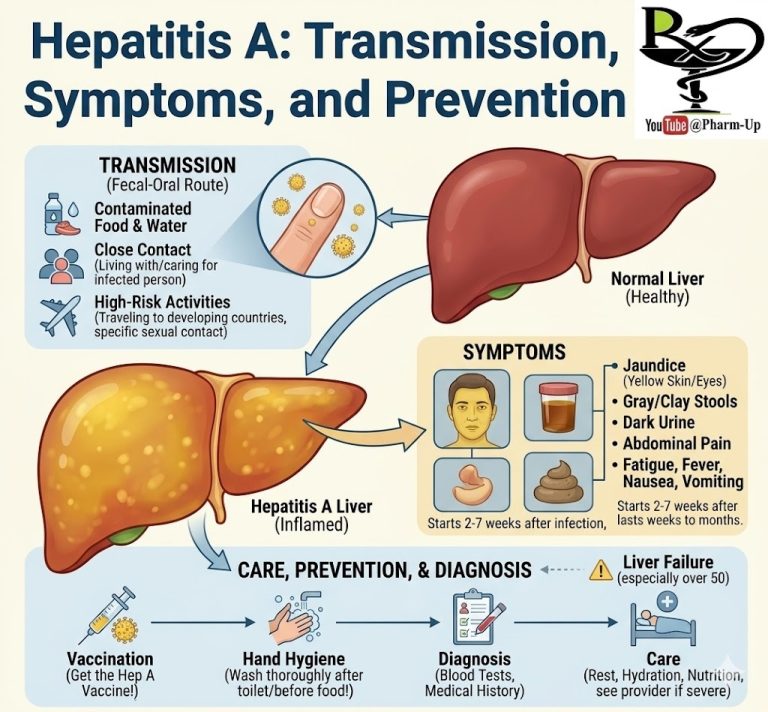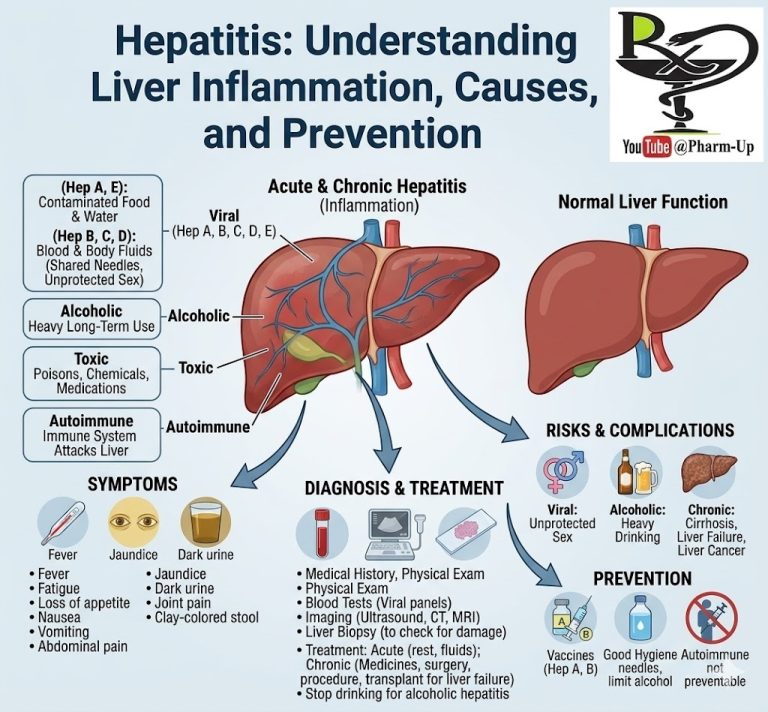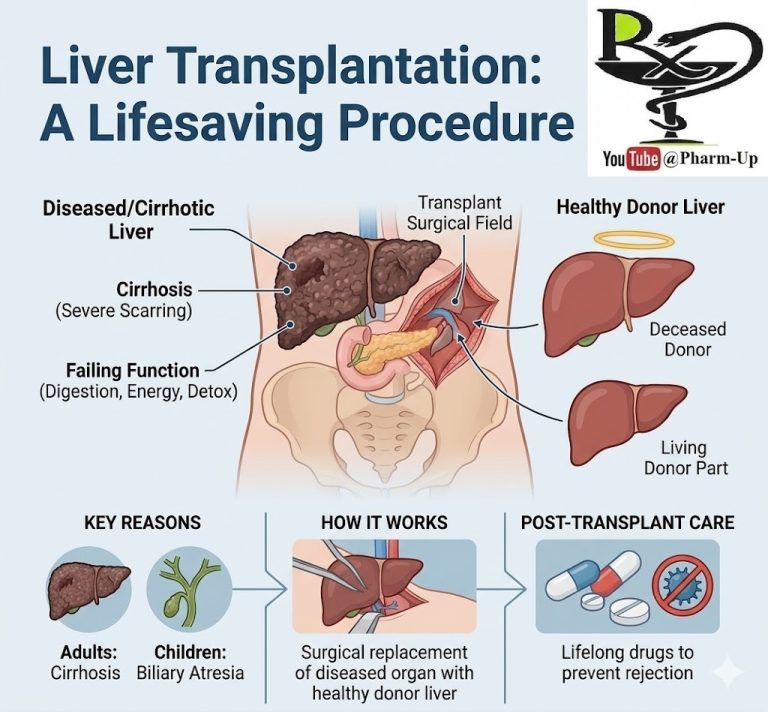
Blood thinners are crucial medications designed to prevent the formation of life-threatening blood clots. Despite their common name, these drugs do not literally “thin” the blood; rather, they interfere with the complex biochemical processes that lead to clotting. Their primary function is to prevent new clots from forming and to stop existing ones from growing larger, thereby reducing the risk of devastating events such as heart attacks, strokes, and pulmonary embolisms.
Why Are Blood Thinners Prescribed?
Blood thinners are a cornerstone of preventive medicine for individuals at high risk of clot formation. Conditions and circumstances that necessitate their use include:
- Abnormal Heart Rhythms: Conditions like atrial fibrillation (AFib), where irregular heartbeats can cause blood to pool and form clots within the heart chambers.
- Heart Valve Conditions: Patients with artificial heart valves, as these can be sites for clot formation.
- Post-Surgical Prevention: After major surgeries, particularly orthopedic procedures like hip or knee replacement, when prolonged immobility increases clot risk.
- History of Clots: Individuals who have experienced deep vein thrombosis (DVT), pulmonary embolism (PE), or a previous stroke/heart attack.
- Congenital Heart Defects: Certain structural heart abnormalities that disrupt normal blood flow.
The Two Main Classes of Blood Thinners
Blood thinners are broadly categorized into two types, each with a distinct mechanism of action:
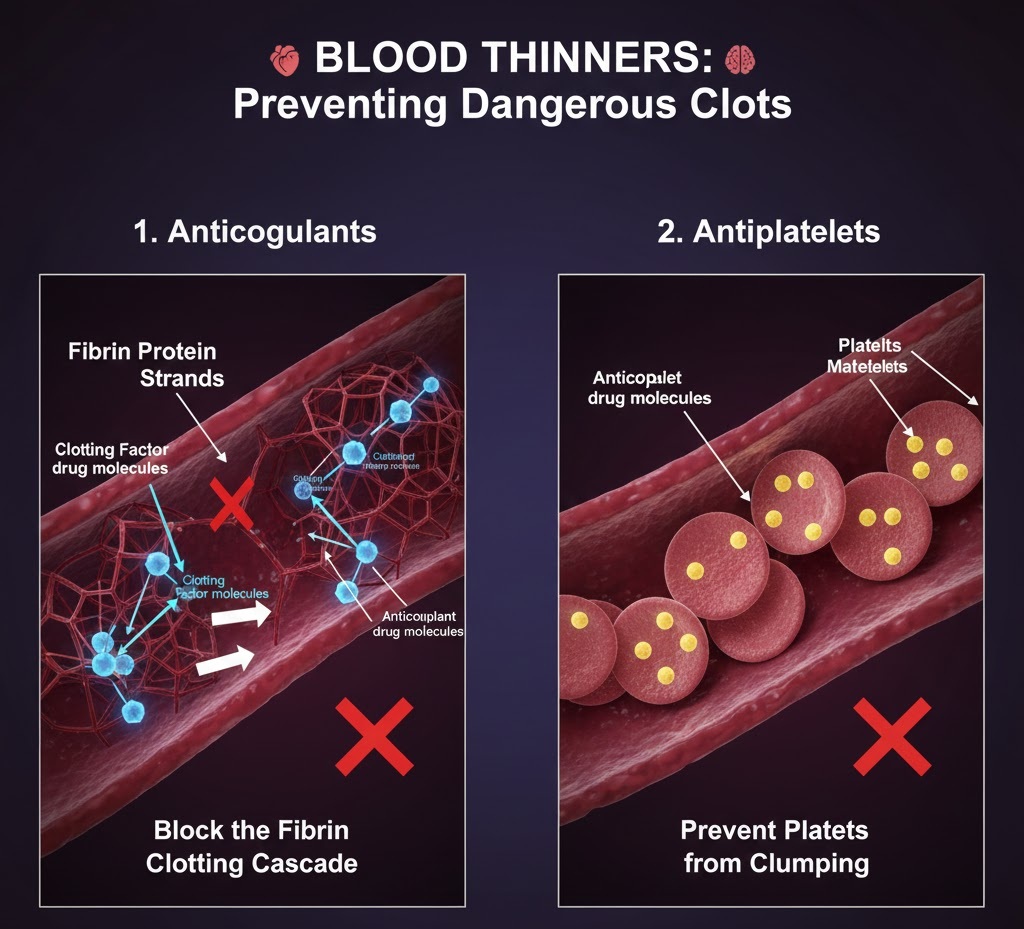
1. Anticoagulants
- Mechanism: These drugs target the body’s coagulation cascade, a series of chemical reactions that result in the formation of fibrin, the mesh-like protein that traps blood cells to form a clot. Anticoagulants slow down or inhibit these chemical reactions.
- Examples:
- Warfarin (Coumadin): An older oral anticoagulant that inhibits Vitamin K-dependent clotting factors. Requires regular monitoring of INR (International Normalized Ratio).
- Heparin: Often given via injection (intravenous or subcutaneous), used for rapid-onset anticoagulation, particularly in hospital settings.
- Direct Oral Anticoagulants (DOACs) / Novel Oral Anticoagulants (NOACs): Such as apixaban (Eliquis), rivaroxaban (Xarelto), and dabigatran (Pradaxa). These directly inhibit specific clotting factors and generally require less frequent monitoring than warfarin.
- Primary Use: Preventing clots in conditions like AFib, DVT, PE, and after heart valve replacement.
2. Antiplatelets
- Mechanism: These medications prevent platelets (tiny blood cells responsible for initial clot formation) from clumping together and adhering to injured blood vessel walls.
- Examples:
- Aspirin: A common antiplatelet often prescribed in low doses for long-term prevention.
- Clopidogrel (Plavix): Frequently used after a heart attack or stroke, or in patients with peripheral artery disease.
- Primary Use: Preventing arterial clots that can lead to heart attacks and strokes, especially in individuals with a history of these events or significant cardiovascular disease.
Safe Usage and Potential Side Effects
The most significant and common side effect of all blood thinners is bleeding. This risk necessitates careful adherence to prescribed dosages and vigilant monitoring.
Important Safety Guidelines:
- Strict Adherence: Take medication exactly as prescribed, at the same time each day.
- Drug Interactions: Inform your healthcare provider about all medications, over-the-counter drugs, herbal supplements, and vitamins (especially Vitamin K, which can affect warfarin) you are taking. Alcohol consumption can also interact with blood thinners.
- Regular Monitoring: For some blood thinners (like warfarin), routine blood tests (e.g., INR) are crucial to ensure the medication level is therapeutic—preventing clots without causing excessive bleeding.
Signs of Serious Bleeding (Seek Immediate Medical Attention):
- Visible Bleeding: Heavy or prolonged menstrual bleeding, blood in urine (red/brown), black or tarry stools, persistent nosebleeds or bleeding gums.
- Internal Bleeding: Severe or unusual headaches or stomachaches, unexpected bruising, or vomiting blood or material resembling coffee grounds.
- Trauma: Any significant fall or head injury, even if seemingly minor, should be reported to a doctor immediately due to increased risk of internal bleeding.
- Systemic Symptoms: Dizziness, weakness, or feeling faint could indicate significant blood loss.