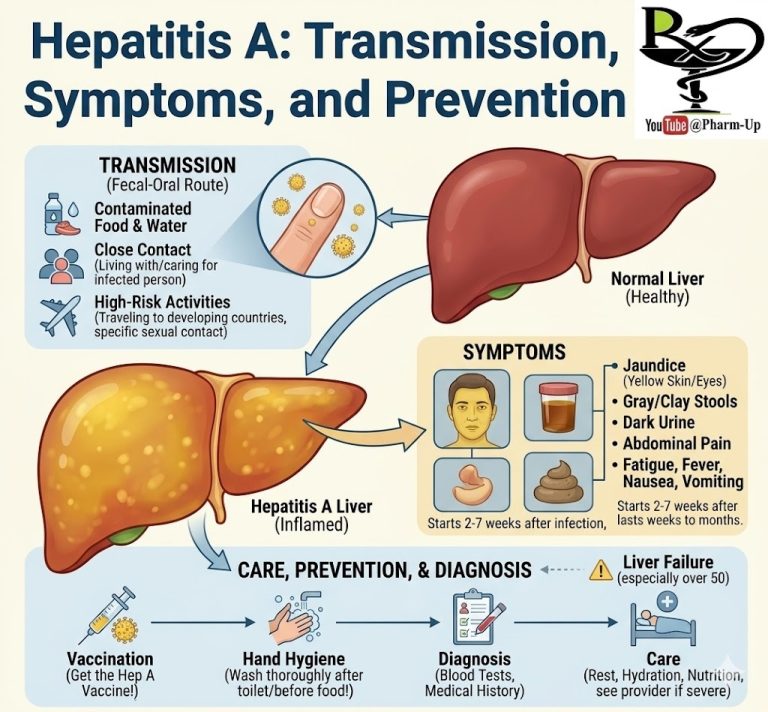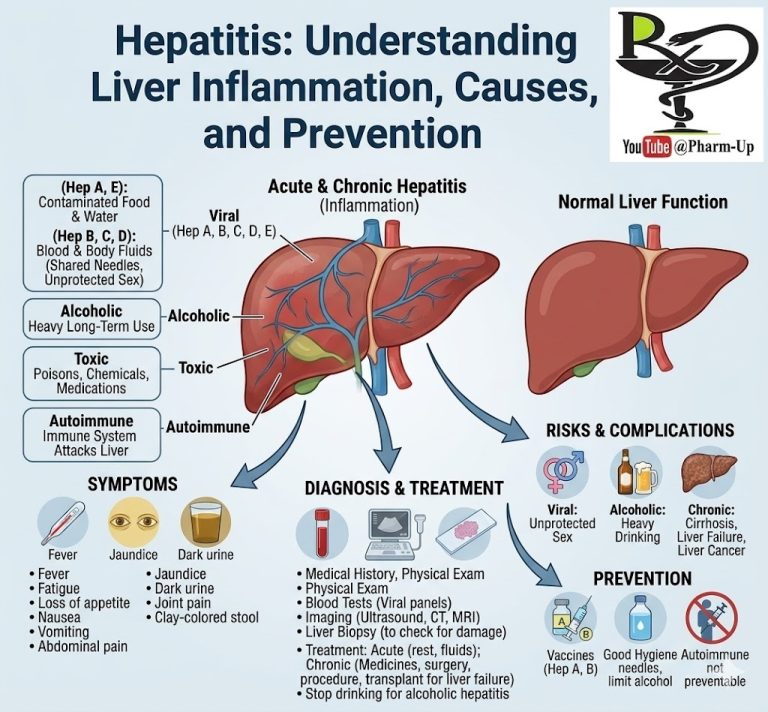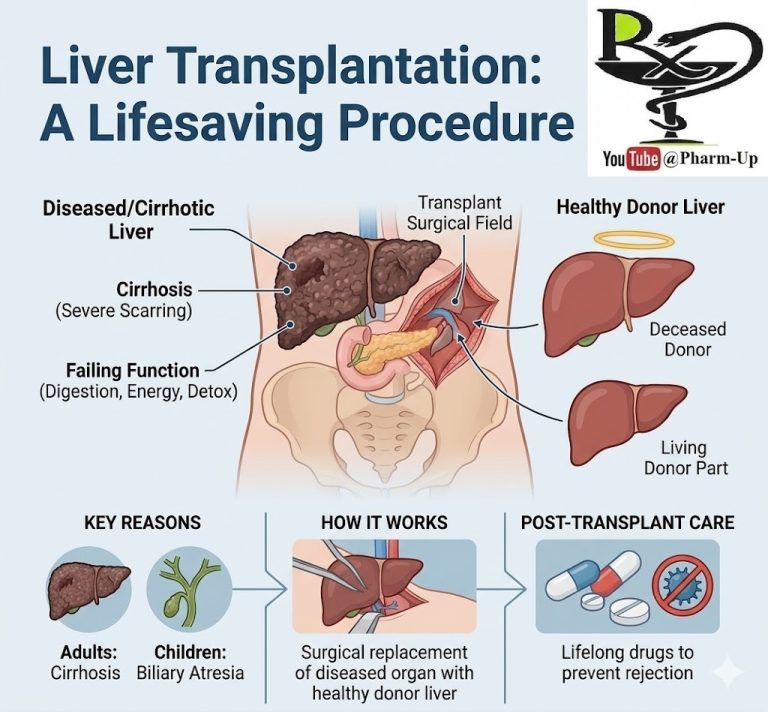
Diabetic neuropathy is a serious and common complication of Type 1 and Type 2 diabetes. It is a type of nerve damage caused by long-term high blood sugar (hyperglycemia). When glucose levels remain elevated, they interfere with the ability of nerves to transmit signals and damage the walls of the small blood vessels (capillaries) that supply the nerves with oxygen and nutrients.
How Nerve Damage Occurs
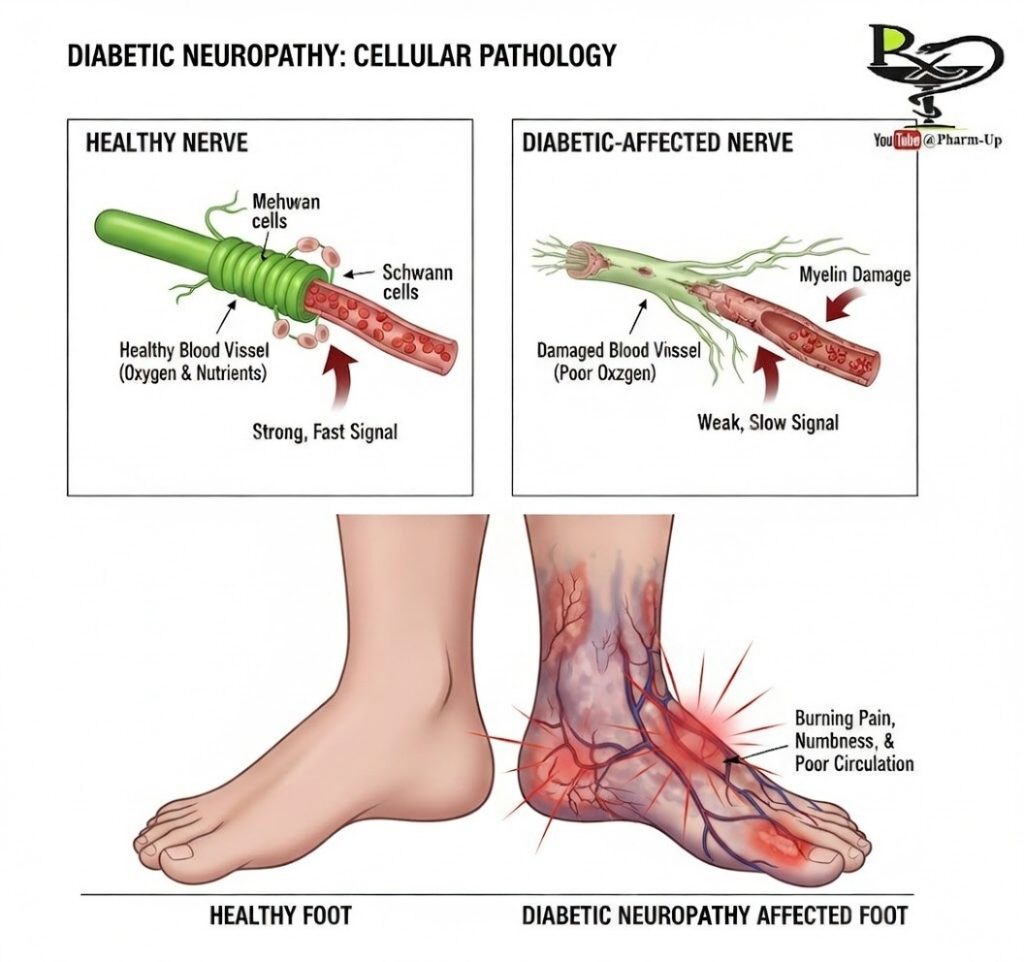
The damage typically happens in two ways:
- Vascular Damage: High sugar weakens the capillary walls, “starving” the nerve of oxygen.
- Structural Damage: The high glucose levels can damage the myelin sheath, which is the protective coating around the nerve fibers.
Common Symptoms and Types
Because nerves run throughout the entire body, symptoms can appear almost anywhere. The most common form is peripheral neuropathy, which affects the feet and legs first, followed by the hands and arms.
- Sensory Symptoms: Burning, tingling (“pins and needles”), shooting pains, or complete numbness.
- Autonomic Symptoms: Damage to nerves that control internal organs can lead to:
- Digestive issues: Nausea, vomiting, or “gastroparesis” (slow stomach emptying).
- Cardiovascular issues: Dizziness or fainting when standing up (orthostatic hypotension).
- Urinary/Sexual issues: Bladder infections or erectile dysfunction.
Diagnosis and Prevention
There is currently no way to reverse nerve damage once it has occurred, which makes early diagnosis and prevention vital.
Diagnostic Tests:
- Filament Testing: Using a soft nylon fiber to test the sensitivity of the feet.
- Nerve Conduction Studies: Measuring how quickly nerves conduct electrical signals.
- Autonomic Testing: Checking how heart rate and blood pressure respond to changes in position.
The Power of Management: The most effective way to manage diabetic neuropathy is tight blood sugar control. Keeping your A1C levels within the target range recommended by your doctor can prevent further damage and, in some cases, improve existing symptoms.