An arrhythmia is a disruption in the rate or rhythm of your heartbeat. While a healthy heart follows a steady, coordinated electrical sequence to pump blood, an arrhythmia occurs when these electrical signals misfire, causing the heart to beat too fast, too slow, or erratically.
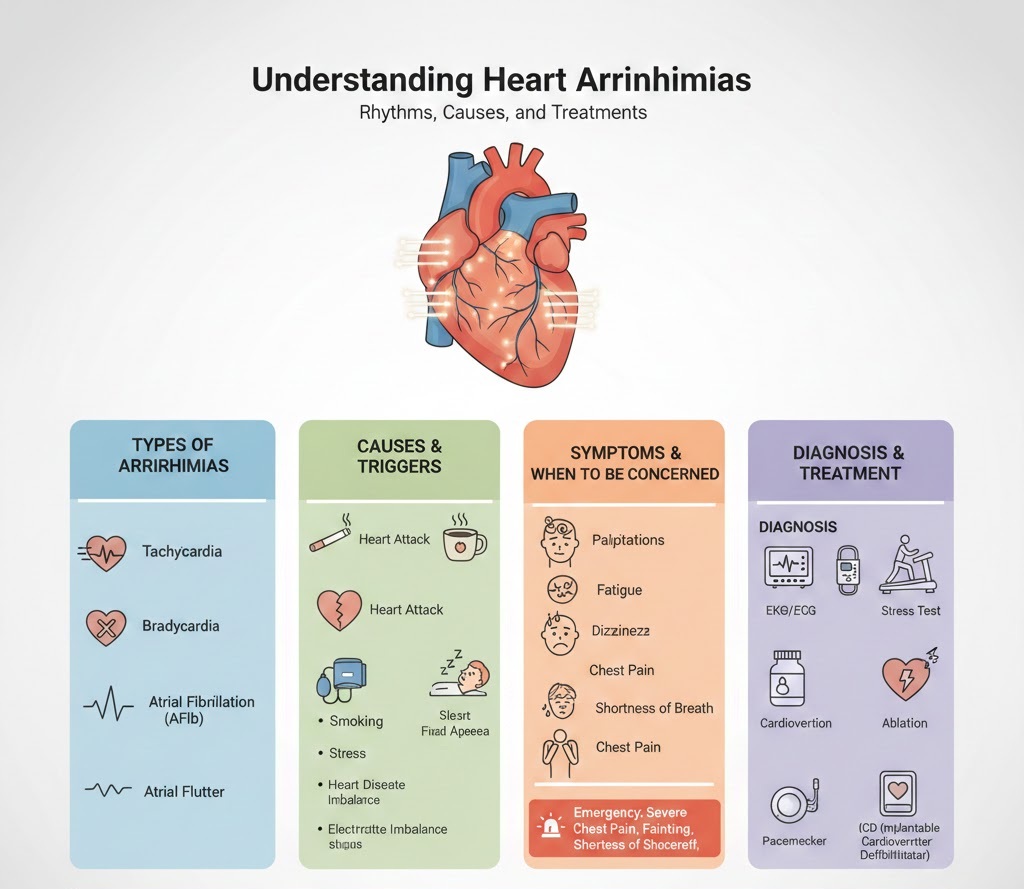
1. Types of Arrhythmias
Arrhythmias are classified by where they originate (atria or ventricles) and the speed of the heart rate.
- Tachycardia: A resting heart rate greater than 100 beats per minute (bpm).
- Bradycardia: A resting heart rate slower than 60 bpm.
- Atrial Fibrillation (AFib): The most common type, characterized by chaotic electrical signals in the upper chambers (atria), leading to an irregular, fast rhythm.
- Atrial Flutter: Similar to AFib but with more organized, “sawtooth” electrical patterns.
- Premature Contractions: Extra beats that feel like a “skipped beat” or a “flip-flop” in the chest.
- Ventricular Fibrillation (V-Fib): A life-threatening emergency where the lower chambers (ventricles) quiver uselessly instead of pumping blood.
2. Common Causes and Triggers
The electrical pathways of the heart can be damaged or interrupted by a variety of internal and external factors:
- Heart Conditions: Previous heart attacks, coronary artery disease, heart valve disorders, or congenital heart defects.
- Lifestyle Factors: Smoking, excessive alcohol or caffeine consumption, and the use of illegal drugs (like stimulants).
- Medical Comorbidities: High blood pressure, sleep apnea, diabetes, thyroid overactivity (hyperthyroidism) or underactivity (hypothyroidism).
- Acute Triggers: Severe stress, electrolyte imbalances (like potassium or magnesium levels), and certain over-the-counter cold and allergy medications.
3. Symptoms: When to Be Concerned
Many arrhythmias are “silent” and only discovered during a routine physical. When symptoms do occur, they typically include:
- Palpitations: A feeling of racing, pounding, or fluttering.
- Fatigue: Feeling unusually tired or weak during light activity.
- Lightheadedness: Dizziness or near-fainting spells (syncope).
- Physical Discomfort: Shortness of breath, chest pain, or sudden sweating.
Emergency Note: If you experience sudden chest pain, severe shortness of breath, or fainting, seek emergency medical services immediately.
4. Diagnosis and Monitoring
To identify the specific rhythm disturbance, healthcare providers use several diagnostic tools:
- Electrocardiogram (EKG/ECG): The gold standard test that records the heart’s electrical signals via sensors on the skin.
- Holter/Event Monitors: Portable devices worn for days or weeks to catch irregular rhythms that don’t happen in the doctor’s office.
- Echocardiogram: An ultrasound used to see if structural heart issues are causing the rhythm problem.
- Stress Test: Monitoring the heart’s rhythm while the patient walks on a treadmill.
5. Treatment Options
The goal of treatment is to control the heart rate and prevent blood clots (which can lead to strokes).
- Medications: Beta-blockers or calcium channel blockers to slow the heart rate, or anti-arrhythmics to restore rhythm.
- Cardioversion: A medical procedure where an electrical shock is delivered to the heart to “reset” it to a normal rhythm.
- Ablation: A catheter-based procedure that uses heat or cold energy to destroy the tiny area of heart tissue causing the erratic signals.
- Implantable Devices:
- Pacemaker: A small device that sends electrical pulses to help the heart beat at a normal rate (used for bradycardia).
- ICD (Implantable Cardioverter Defibrillator): A device that monitors rhythm and delivers a shock if a life-threatening rhythm is detected.
6. Prevention and Lifestyle
You can reduce your risk by maintaining a heart-healthy lifestyle:
- Engage in regular physical activity.
- Eat a diet rich in fruits, vegetables, and lean proteins.
- Manage stress through mindfulness or therapy.
- Monitor blood pressure and cholesterol levels regularly.