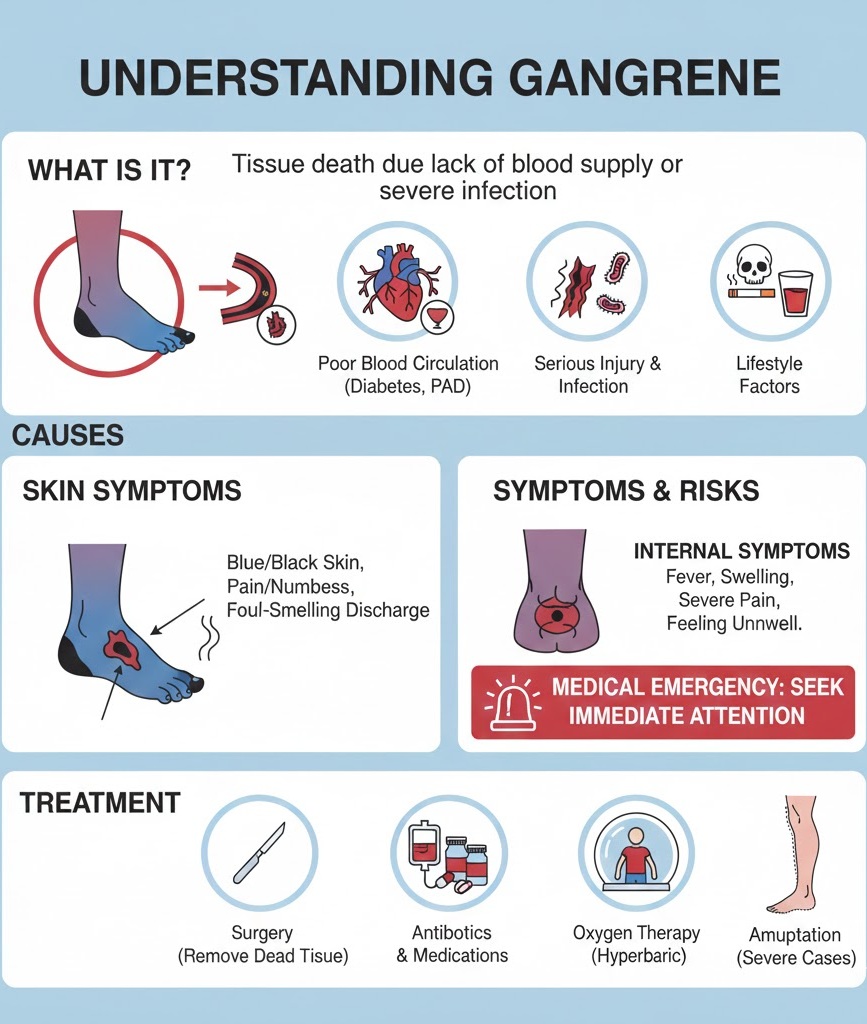
Gangrene is a life-threatening condition characterized by the death of body tissue. It occurs when a specific area of the body loses its blood supply, depriving cells of the oxygen and nutrients they need to survive. This can happen on the skin’s surface or within deep tissues, muscles, and internal organs.
Key Causes
The primary trigger for gangrene is a lack of blood flow or a severe infection. Common risk factors include:
- Poor Blood Circulation: Long-term conditions like diabetes, atherosclerosis (hardened arteries), and peripheral arterial disease significantly increase risk.
- Traumatic Injury: Serious wounds, burns, or frostbite that damage blood vessels.
- Infection: Bacteria (especially in “gas gangrene”) can release toxins that kill surrounding tissue.
Recognizing the Symptoms
Symptoms vary depending on whether the gangrene is “dry” (circulation-related) or “wet” (infection-related):
- Skin Changes: The area may turn blue, purple, or black.
- Sensation: Initial severe pain followed by a loss of feeling or numbness.
- Discharge: Sores may develop that produce a foul-smelling fluid or pus.
- Internal Signs: If gangrene is inside the body (such as the gallbladder or appendix), symptoms include high fever, swelling, and a general feeling of being very unwell.
Treatment Options
Gangrene is a medical emergency. Immediate hospitalization is required to stop the spread of tissue death.
- Surgery (Debridement): Doctors remove the dead tissue to prevent the infection from spreading to healthy areas.
- Antibiotics: Delivered intravenously to fight bacterial infections.
- Oxygen Therapy (Hyperbaric): In some cases, patients are placed in a high-pressure oxygen chamber to help saturated tissues heal and kill anaerobic bacteria.
- Amputation: In severe cases where the damage is too extensive to save the limb, amputation may be necessary to save the person’s life.