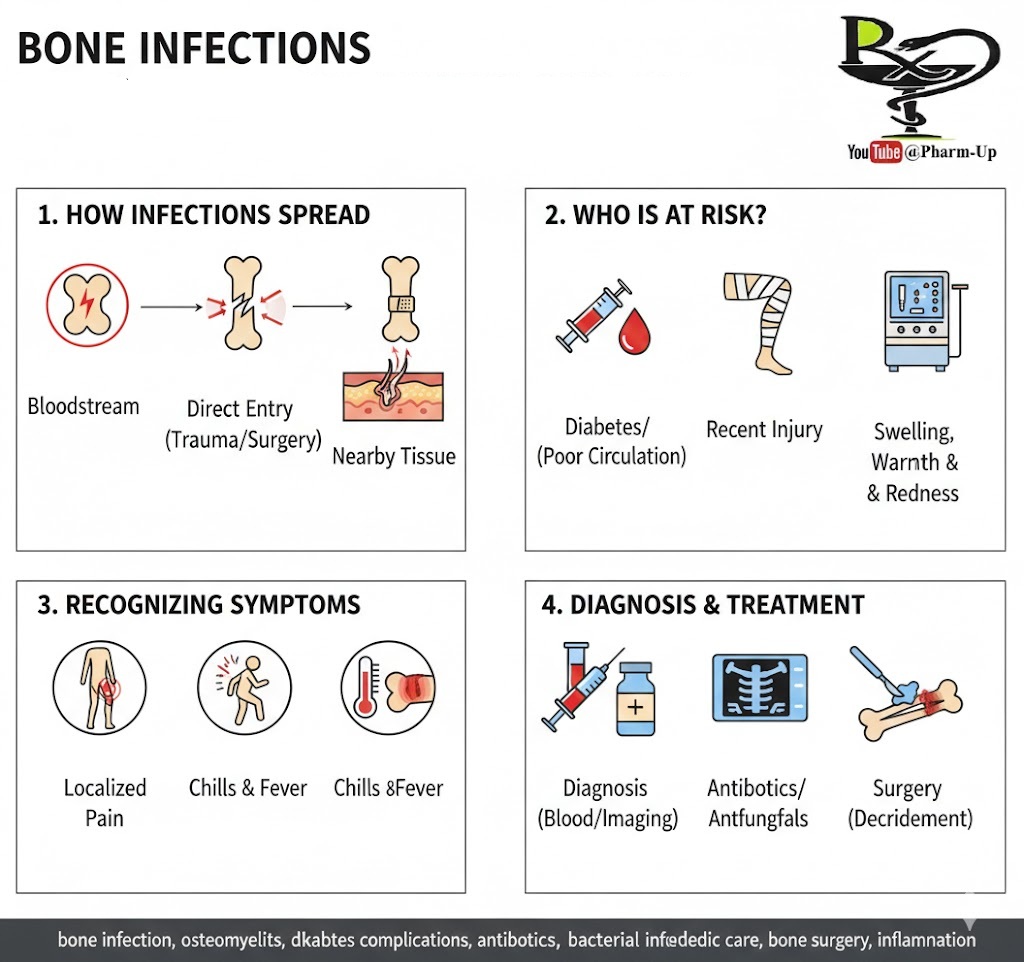
A bone infection, medically known as osteomyelitis, occurs when bacteria or fungi invade the bone tissue. While bones are generally resistant to infection, certain conditions can allow pathogens to take hold, leading to inflammation and potential bone damage.
1. How Infections Reach the Bone
Pathogens can enter the skeletal system through three primary routes:
- The Bloodstream: An infection in another part of the body (like the lungs or urinary tract) can travel through the blood to a weak spot in a bone.
- Direct Entry: A deep wound, an open fracture, or a recent surgery can expose the bone directly to germs.
- Nearby Tissue: Infections in the skin or muscles (such as a deep pressure sore) can spread into the underlying bone.
2. Who Is at Risk?
Certain factors make it harder for the body to fight off bone-seeking pathogens:
- Diabetes & Poor Circulation: Reduced blood flow prevents immune cells from reaching the site of an injury.
- Recent Trauma: Broken bones or deep puncture wounds.
- Hemodialysis: Frequent use of needles for blood filtration can increase the risk of bacteria entering the bloodstream.
- Weakened Immune Systems: Those undergoing chemotherapy or living with chronic illnesses.
3. Recognizing the Symptoms
Early detection is vital to prevent permanent bone loss. Look for:
- Localized Pain: Deep, aching pain in the infected area.
- Visible Signs: Swelling, warmth, and intense redness over the bone.
- Systemic Signs: Chills, high fever, and a general feeling of fatigue.
4. Diagnosis and Treatment
Doctors typically use a combination of blood tests (to check for high white blood cell counts) and imaging (like X-rays, CT scans, or MRIs) to confirm the diagnosis.
- Antibiotics/Antifungals: Usually administered through an IV for several weeks to ensure the infection is completely eradicated.
- Surgery: In many cases, a surgeon must perform “debridement” to remove the dead or infected part of the bone so the healthy tissue can heal.