Osteoarthritis (OA) is a joint disease that primarily affects the hands, knees, hips, neck, and lower back. Unlike other forms of arthritis, OA specifically targets the joint structure rather than the immune system.
1. What Happens in the Joint?
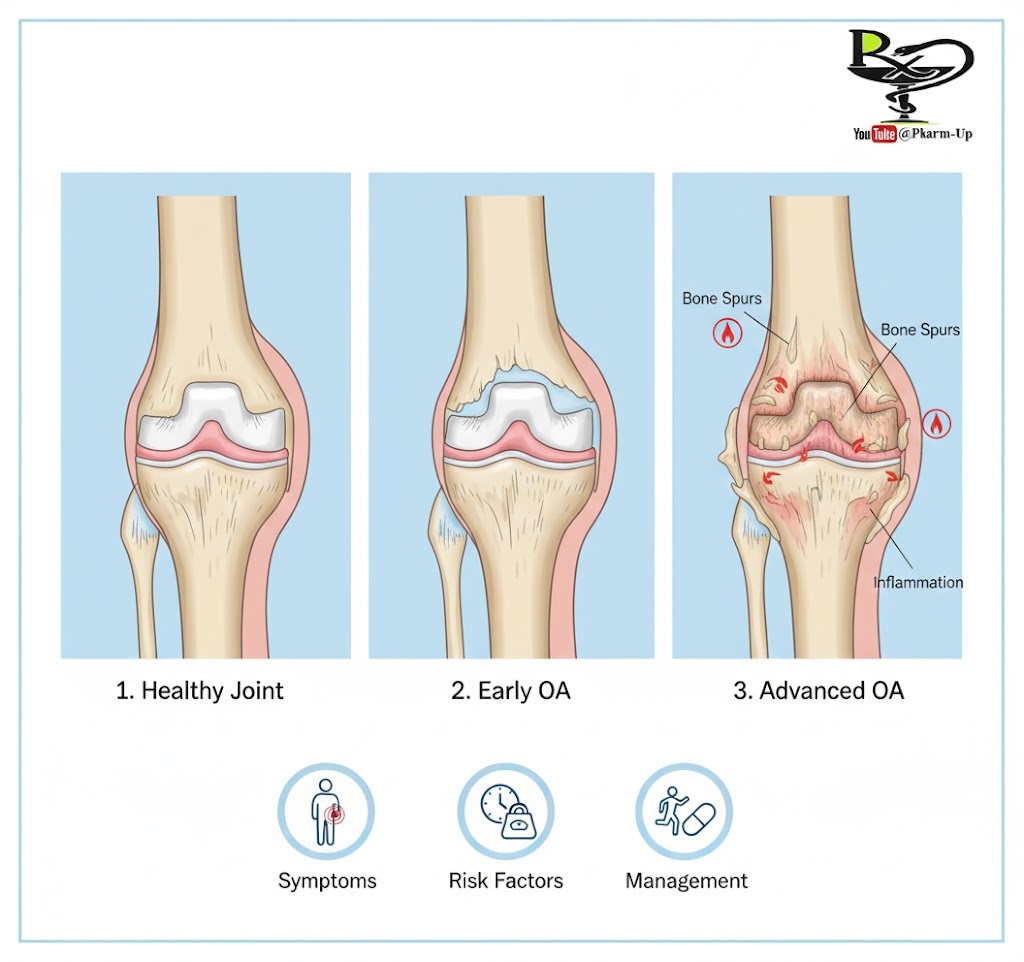
In a healthy joint, the ends of your bones are capped with cartilage—a smooth, slippery tissue that acts as a shock absorber and allows bones to glide against each other.
- Cartilage Breakdown: In OA, this cartilage becomes rough and wears down.
- Bone-on-Bone Friction: If the cartilage wears away completely, the bones rub directly against each other.
- Bone Spurs: The body may try to repair the damage by growing extra bumps of bone, called spurs, in the joint area.
2. Symptoms to Watch For
Osteoarthritis affects everyone differently, and symptoms often develop slowly over time:
- Movement Pain: Aching during activity that typically improves with rest.
- Morning Stiffness: Joint stiffness that lasts for about 30 minutes after waking up.
- Swelling: Occurs frequently after heavy use of the joint.
- Reduced Mobility: Feeling that the joint is less flexible or “loose/unstable.”
3. Risk Factors: Who is Most Likely to Develop OA?
While the exact cause is a mix of environmental and biological factors, certain things increase your risk:
- Aging: Risk increases significantly after age 50 (especially in women).
- Weight: Extra body weight places mechanical stress on the hips and knees.
- Joint History: Past injuries, surgeries, or joints that are misaligned.
- Overuse: Repetitive motions from sports (jumping, twisting) or specific jobs.
- Genetics: A family history of the condition.
4. Diagnosis and Management
There is no single test for OA. Providers use medical history, physical exams, and X-rays to see if cartilage loss or bone spurs are present.
Treatment Goals
Since there is no cure, treatment focuses on reducing pain and maintaining movement:
- Lifestyle: Strengthening exercises, balance training, and weight loss.
- Support: Custom braces or shoe inserts (orthotics).
- Medication: Over-the-counter creams/pills, or prescription injections for severe cases.
- Complementary Care: Heat/ice therapy, massage, or acupuncture.
- Surgery: A final option if conservative treatments fail to provide relief.