Walking is a highly coordinated activity involving the brain, spinal cord, nerves, muscles, and bones. When one of these systems is disrupted, it changes your gait—the specific pattern of how you walk. Understanding these changes is the first step toward regaining mobility and safety.
Recognizing Abnormal Gait Patterns
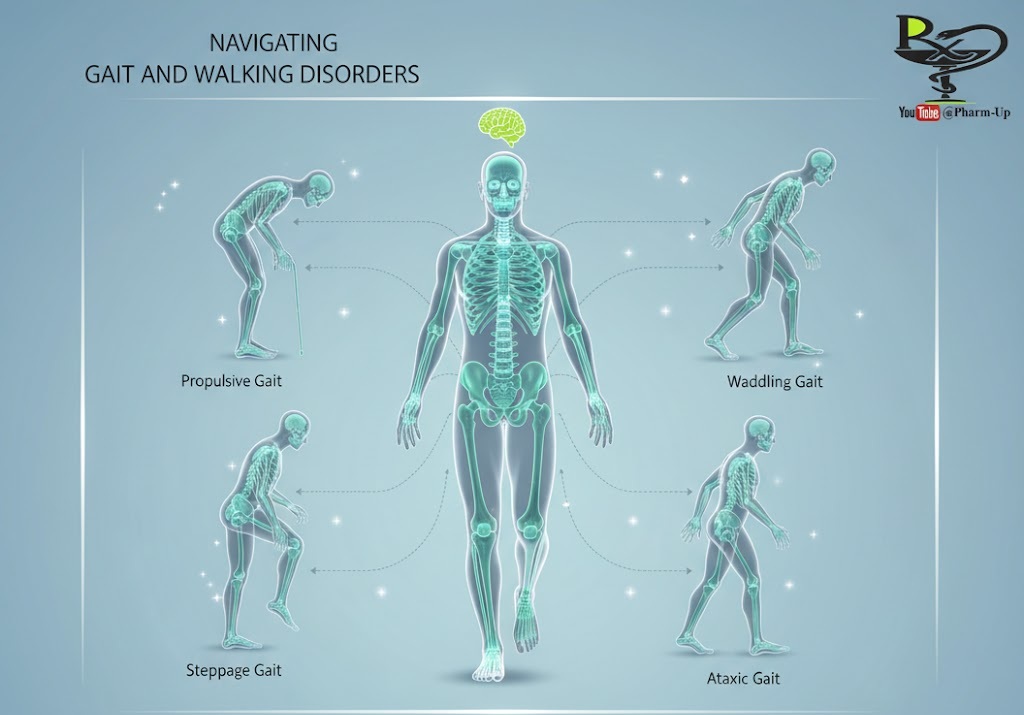
Walking problems often manifest in specific ways that can help healthcare providers identify the underlying cause:
- Propulsive Gait: A stooped, stiff posture with the head and neck bent forward.
- Steppage Gait: Lifting the leg unusually high to prevent a “dropped” foot from dragging on the ground.
- Waddling Gait: A duck-like walk that may indicate hip weakness or bone development issues.
- Ataxic Gait: Unsteady, uncoordinated walking with a wide base, often linked to cerebellar (balance center) issues.
The Root Causes of Mobility Issues
Because walking is a “total body” event, the causes of dysfunction are diverse:
| Category | Examples |
| Neurological | Parkinson’s disease, Multiple Sclerosis, or peripheral nerve damage. |
| Structural | Arthritis in the knees or hips, bone fractures, and leg length discrepancies. |
| Acute Injury | Severe sprains, tendinitis, or muscle strains. |
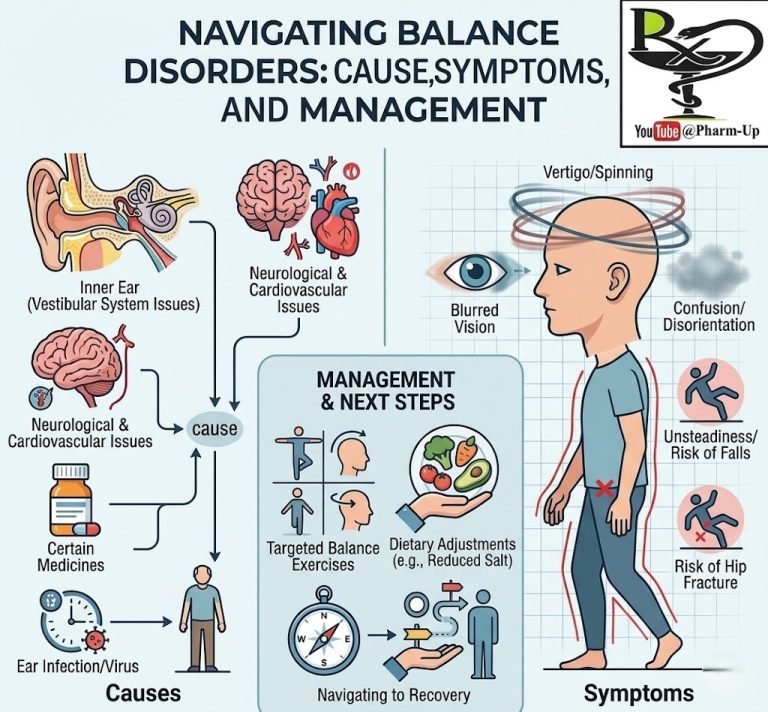
| Sensory | Vision impairment or inner ear issues that affect balance. |
Diagnosis and Path to Recovery
A diagnosis usually begins with a Gait Analysis, where a provider observes your movement, stride length, and posture.
- Neurological Exam: Checking reflexes and muscle tone.
- Imaging: X-rays or MRIs to look for joint degeneration or nerve compression.
- Treatment: This may range from Physical Therapy (to strengthen muscles) and Mobility Aids (canes/walkers) to Orthotics (custom shoe inserts) or corrective surgery.