Sjögren’s (pronounced SHOW-grins) syndrome is a chronic autoimmune disorder where the body’s immune system mistakenly attacks its own moisture-producing glands. While it is primarily known for causing systemic dryness, it is a complex condition that can affect multiple organ systems.
Primary vs. Secondary Sjögren’s
- Primary Sjögren’s: Occurs on its own without another underlying rheumatic disease.
- Secondary Sjögren’s: Develops alongside another autoimmune condition, most commonly Rheumatoid Arthritis or Lupus.
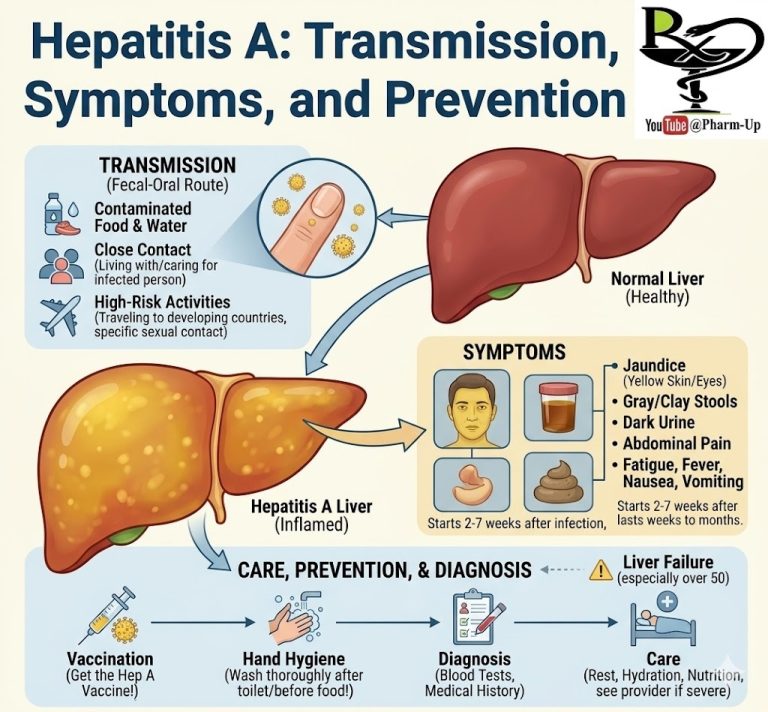
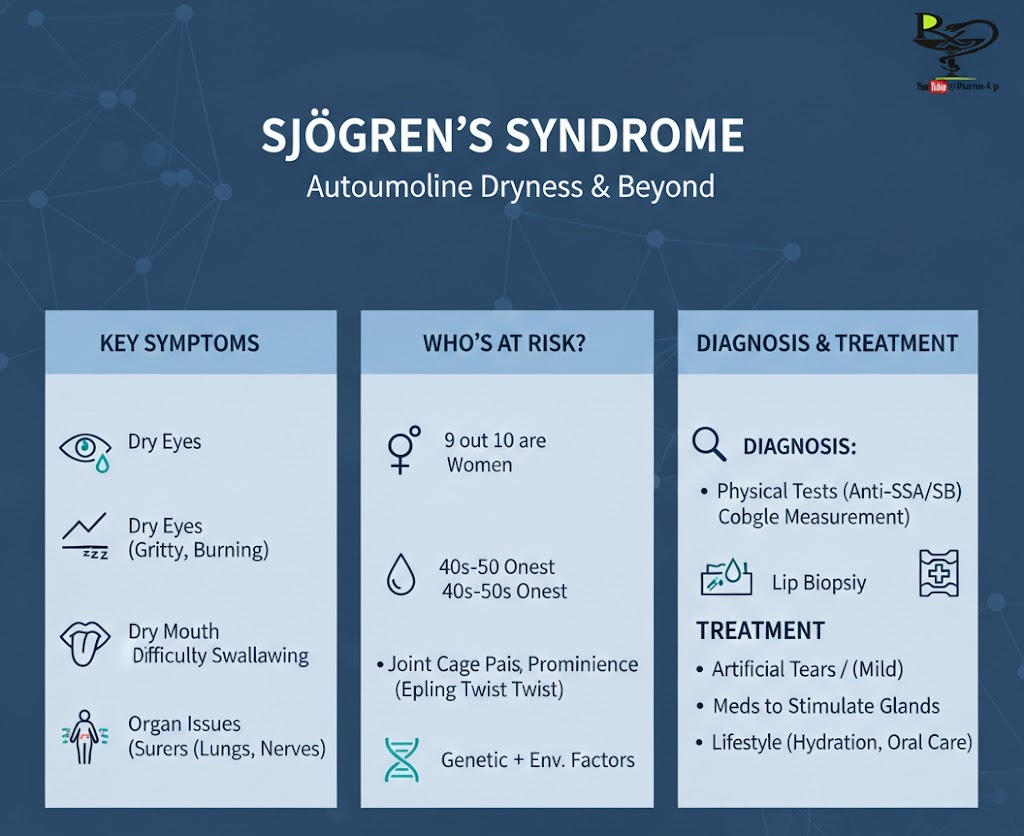
Key Symptoms: The “Sicca” Complex
The hallmark symptoms revolve around “Sicca” (dryness), but the disease often extends further:
- Dry Eyes: A persistent gritty, burning, or “sandy” sensation. Eyes may be sensitive to light or appear red.
- Dry Mouth (Xerostomia): A “cotton-mouthed” feeling that makes it difficult to swallow dry foods, speak for long periods, or taste.
- Systemic Effects:
- Joint/Muscle Pain: Similar to arthritis.
- Profound Fatigue: A heavy, lingering tiredness that rest doesn’t fix.
- Organ Involvement: Inflammation can affect the lungs (chronic cough), kidneys, and nerves (numbness/tingling).
- Dental Issues: Lack of saliva leads to a rapid increase in dental cavities and gum disease.
Who is at Risk?
- Gender: Roughly 9 out of 10 patients are women.
- Age: It can affect anyone, but diagnosis usually occurs in the 40s or 50s.
- Genetics & Environment: While not directly inherited, certain genes make people more susceptible, often triggered by a viral or bacterial infection.
Diagnosis and Management
Diagnosis
Because symptoms overlap with many other conditions, doctors use a combination of:
- Schirmer’s Test: A small strip of paper is placed in the eyelid to measure tear production.
- Lip Biopsy: Taking a tiny sample of minor salivary glands to look for characteristic inflammation.
- Blood Work: Looking for specific antibodies like Anti-SSA (Ro) and Anti-SSB (La).
Treatment & Self-Care
There is no cure, so management focuses on moisture replacement and inflammation control:
- Moisture Replacement: Artificial tears, eye ointments, and saliva substitutes.
- Stimulants: Prescription meds (like pilocarpine) to “force” glands to produce more moisture.
- Punctal Plugs: Tiny plugs inserted into tear ducts to keep natural tears on the eye surface longer.
- Lifestyle: Sip water frequently, use sugar-free gum/candy, use humidifiers, and maintain strict dental hygiene.