Juvenile arthritis (JA) is an umbrella term for several autoimmune conditions that cause joint inflammation in children under the age of 16. Unlike adult arthritis, JA can uniquely impact a child’s physical development, growth, and even internal organs, making early diagnosis and specialized care essential.
Understanding Juvenile Idiopathic Arthritis (JIA)
The most common form of JA is Juvenile Idiopathic Arthritis. The term “idiopathic” means the exact cause is unknown, though it is categorized as an autoimmune disorder where the immune system mistakenly attacks healthy joint tissues.
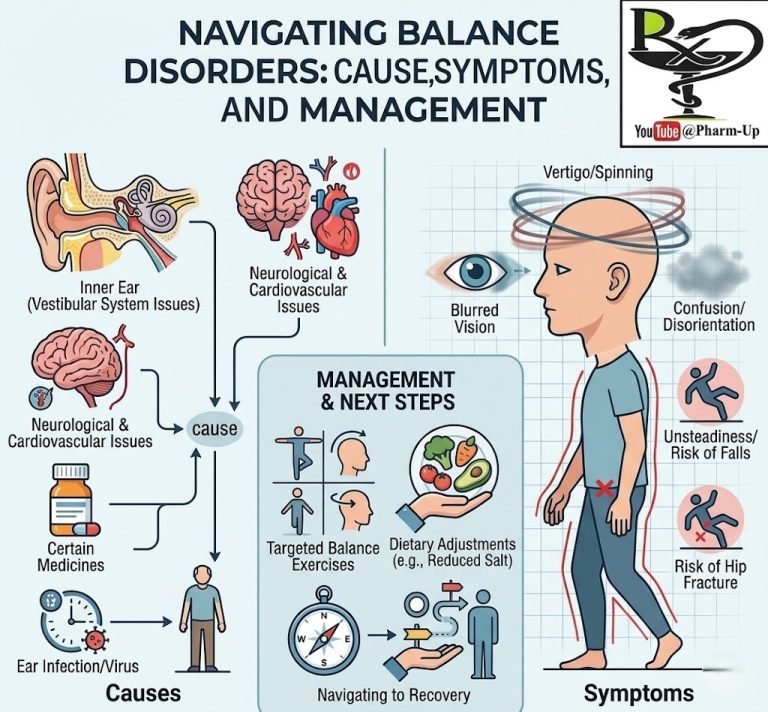
- Early Indicators: Children may not always complain of pain. Parents should look for morning limping, unusual clumsiness after naps, or visible swelling in large joints like the knees.
- Systemic Symptoms: Beyond joints, some children may experience high fevers, skin rashes, or inflammation of the eye (uveitis), which requires regular check-ups with an ophthalmologist.
The Challenges of Diagnosis
Because there is no single “JA test,” healthcare providers use a combination of tools to rule out other injuries or infections:
- Medical History: Tracking the frequency and timing of stiffness.
- Blood Tests: Checking for inflammatory markers and auto-antibodies.
- Imaging: Using X-rays or MRIs to monitor bone growth and joint space.
Comprehensive Treatment Goals
Management is a team effort involving pediatric rheumatologists, physical therapists, and parents.
| Treatment Component | Purpose |
| Medication | Biologics or NSAIDs to calm the immune system and reduce pain. |
| Physical Therapy | Specialized exercises to maintain range of motion and muscle strength. |
| Growth Monitoring | Ensuring the disease or medications do not interfere with bone development. |
| Eye Care | Routine screenings to prevent vision loss from internal eye inflammation. |