A comprehensive study from Mayo Clinic, published in the Annals of Surgical Oncology, has provided critical insights into the factors that determine long-term survival for patients with HER2-positive breast cancer undergoing neoadjuvant chemotherapy (NAC). The research, which analyzed a large dataset of over 57,000 patients, definitively establishes that a patient’s clinical stage at the time of diagnosis is a paramount predictor of both treatment response and overall survival (OS).
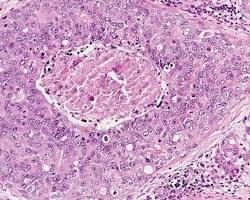
HER2-positive breast cancer is a subtype that accounts for approximately 20% of all breast cancer diagnoses and is known for its aggressive nature and higher risk of recurrence. While NAC has emerged as an effective therapeutic strategy, the precise relationship between a patient’s disease stage, their response to NAC, and their long-term prognosis has been an area of limited understanding in clinical practice.
The study’s findings reveal a powerful correlation: patients diagnosed at an earlier stage have significantly better outcomes, especially when they achieve a pathologic complete response (pCR)—the complete disappearance of all cancer cells in the breast and lymph nodes following chemotherapy.
Key Survival Metrics and Stage-Specific Outcomes:
- For patients who achieved pCR, the 5-year OS rates were exceptionally high across all stages, yet a clear disparity was evident:
- Stage 1: 98% OS
- Stage 2: 97% OS
- Stage 3: 91% OS
- For patients with residual disease (cancer remaining after NAC), the survival rates were notably lower and declined sharply with advancing stage:
- Stage 1: 95% OS
- Stage 2: 91% OS
- Stage 3: 80% OS
The study’s multivariable analysis further underscored the significance of disease stage. While a pCR is a powerful positive prognostic factor, it does not completely erase the risk associated with advanced disease. For example, a patient with a Stage 3 tumor who achieved a pCR had an OS outcome that was still significantly worse than a patient with a Stage 1 tumor who had residual disease.
These results have profound implications for clinical practice and patient care. They confirm that early detection and diagnosis remain the most critical factors for improving long-term outcomes in HER2-positive breast cancer. The findings also highlight the need for tailored, stage-specific treatment strategies. While achieving a pCR is a major goal of NAC, the research suggests that for patients with advanced-stage disease, additional therapeutic interventions may be necessary to fully mitigate their elevated risk and improve their long-term survival. This study provides a crucial roadmap for guiding both prognosis and treatment planning in the management of HER2-positive breast cancer.