Angina is not a disease itself, but rather a warning sign or symptom of an underlying heart problem—most commonly Coronary Artery Disease (CAD). It occurs when your heart muscle (myocardium) doesn’t receive enough oxygen-rich blood, a condition known as ischemia. This lack of oxygen causes the heart to signal distress through pain or pressure.
1. How Angina Feels: The Symptoms
Angina is often described as more than just “pain.” Many people experience it as:
- Pressure or Squeezing: A feeling like an elephant is sitting on your chest or a tight band is being wrapped around it.
- Referred Pain: The discomfort often radiates to the shoulders, arms (especially the left), neck, jaw, or back.
- Atypical Sensations: Some people, particularly women and older adults, may experience it as indigestion, shortness of breath, nausea, or extreme fatigue rather than sharp pain.
2. The Three Primary Types of Angina
Understanding the type of angina is critical because it determines the level of medical urgency.
| Type | Characteristics | Trigger | Relief |
| Stable Angina | Follows a predictable pattern; lasts a short time (5 mins or less). | Physical exertion, emotional stress, or heavy meals. | Rest or Nitroglycerin (medicine). |
| Unstable Angina | Medical Emergency. Unexpected; may be more severe or last longer (20+ mins). | Can occur even while resting or sleeping. | Does not go away with rest or standard medicine. |
| Variant (Prinzmetal) Angina | Rare; caused by a spasm in the coronary artery rather than a blockage. | Usually occurs at rest or during the night/early morning. | Responds well to specific medications. |
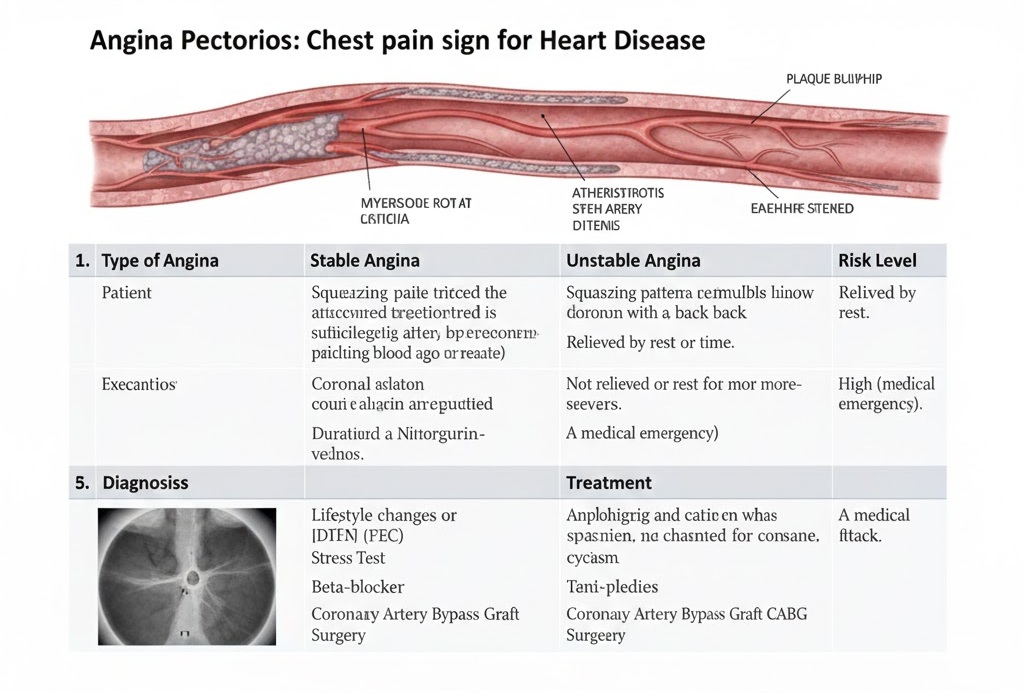
3. Causes: The Plaque Factor
The most common cause of angina is Atherosclerosis.
- Plaque Build-up: Cholesterol, fats, and other substances form “plaque” on the inner walls of the coronary arteries.
- Narrowing: This plaque narrows the arteries over time, restricting blood flow.
- Demand vs. Supply: When you exercise or feel stressed, your heart demands more oxygen. If the narrowed arteries cannot supply it, angina occurs.
4. Diagnosis and Risk Management
If you experience chest pain, healthcare providers use several methods to evaluate the heart:
- EKG (Electrocardiogram): To check for signs of past or current ischemia.
- Stress Test: To see how the heart performs under physical demand.
- Cardiac Catheterization: A procedure to visualize blockages using dye and X-rays.
Risk Factors include: High blood pressure, high cholesterol, smoking, diabetes, obesity, and a sedentary lifestyle.
5. Treatment and Lifestyle
The goal is to reduce the frequency of symptoms and prevent a heart attack.
- Medications: Nitrates (to widen blood vessels), Beta-blockers (to slow heart rate), and Statins (to lower cholesterol).
- Procedures: Angioplasty (stenting) or Coronary Artery Bypass Grafting (CABG) for severe blockages.
- Lifestyle Changes: Quitting smoking, adopting a Mediterranean-style diet, and managing stress.
Emergency Warning: If you have new, worsening, or persistent chest pain that does not go away with rest, call emergency services immediately, as this may be a heart attack.