Angioplasty, also known as Percutaneous Coronary Intervention (PCI), is a minimally invasive procedure designed to open clogged heart arteries. It is a critical tool for treating both chronic heart disease and acute emergencies like heart attacks.
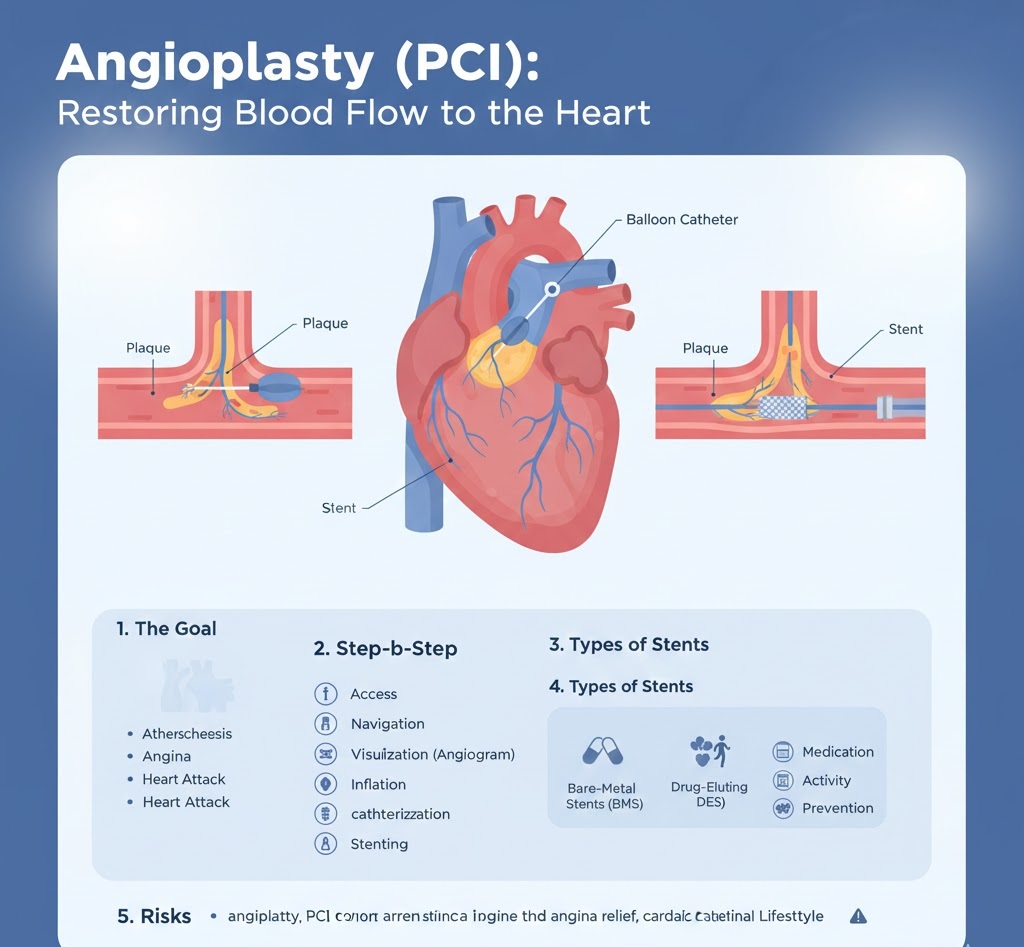
1. The Goal: Overcoming Atherosclerosis
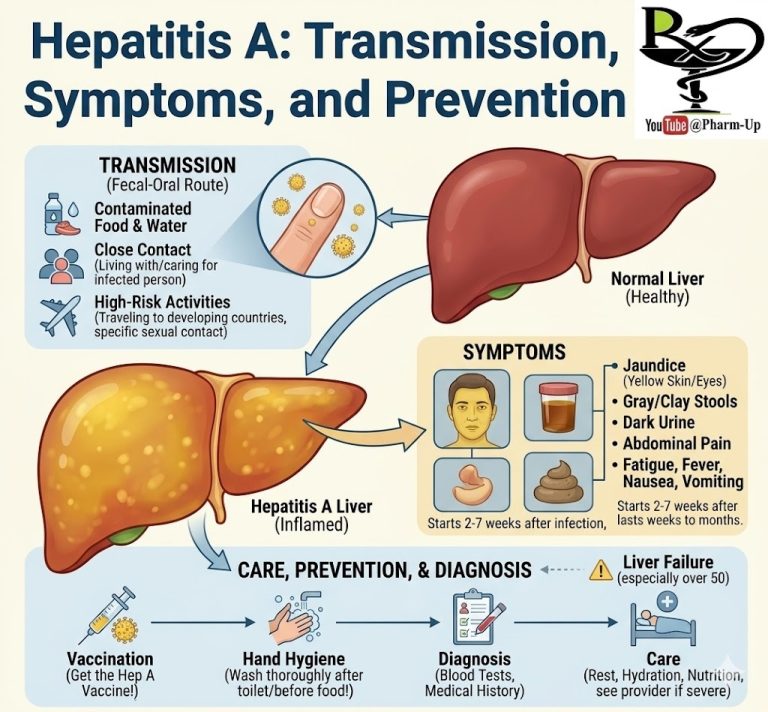
The procedure targets Coronary Artery Disease (CAD). CAD occurs when plaque (a mix of fat, cholesterol, and calcium) builds up on the inner walls of the arteries that feed the heart.
- The Problem: Narrowed arteries restrict oxygen-rich blood, causing angina (chest pain).
- The Danger: If a plaque ruptures, a blood clot can form, completely blocking the artery and causing a heart attack.
2. Step-by-Step: How Angioplasty is Performed
The procedure takes place in a Cardiac Catheterization Lab (Cath Lab). While you are awake but sedated, the cardiologist follows these steps:
- Access: A small incision is made in the wrist (radial artery) or groin (femoral artery).
- Navigation: A thin, flexible tube called a catheter is threaded through the blood vessels until it reaches the opening of the coronary arteries.
- Visualization: Contrast dye is injected, and X-ray images (angiogram) are taken to pinpoint the exact location of the blockage.
- Inflation: A second catheter with a tiny balloon at the tip is guided into the blockage. The balloon is inflated, compressing the plaque against the artery wall.
- Stenting: In most cases, a small metal mesh tube called a stent is expanded at the site to act as a permanent scaffold, keeping the artery open.
3. Types of Stents
Most modern angioplasties involve placing a stent. There are two primary types:
- Bare-Metal Stents (BMS): Simple mesh tubes that provide structural support.
- Drug-Eluting Stents (DES): These are coated with medication that is slowly released to prevent the artery from scarring and narrowing again (a process called restenosis).
4. Recovery and Life After Angioplasty
While angioplasty opens the “pipe,” it does not “cure” the underlying disease. Recovery involves:
- Medication: You will likely need “dual antiplatelet therapy” (such as Aspirin and Clopidogrel) to prevent blood clots from forming on the new stent.
- Activity: Most patients can return to work and light activity within a week, though emergency patients may require more time.
- Prevention: Success depends on managing risk factors through a heart-healthy diet, smoking cessation, and exercise.
5. Risks and Considerations
Though highly common and generally safe, potential risks include:
- Bleeding or bruising at the insertion site.
- Damage to the artery or a sudden closure of the vessel.
- Kidney issues (temporary) from the contrast dye.
- Blood clots forming within the stent.