An aneurysm is a localized, balloon-like bulge in the wall of a blood vessel. This weakening occurs because the pressure of blood flowing through a compromised artery forces the wall to stretch outward. While some aneurysms remain stable for years, others can expand and rupture, leading to life-threatening internal hemorrhaging.
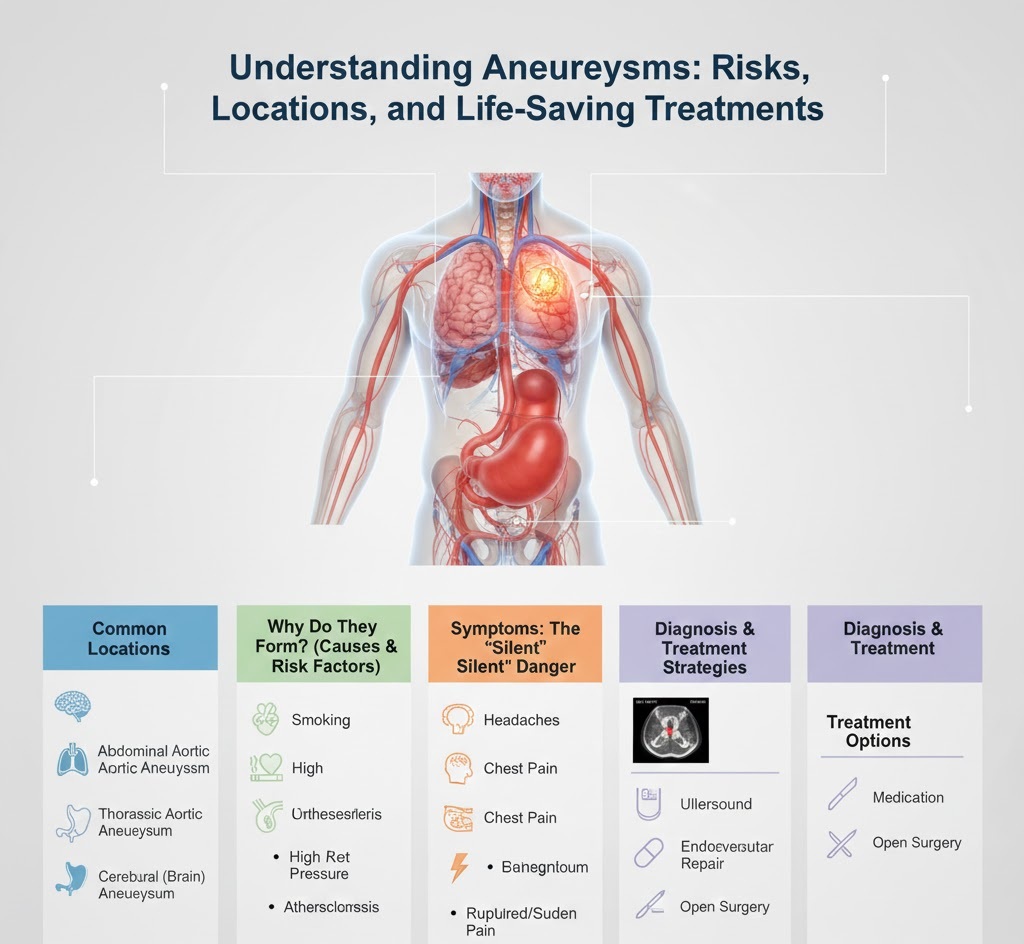
1. Common Locations of Aneurysms
Aneurysms can form anywhere in the arterial system, but they are most dangerous in the following areas:
- Abdominal Aortic Aneurysm (AAA): Occurs in the part of the aorta that passes through the abdomen. This is the most common site for a life-threatening rupture.
- Thoracic Aortic Aneurysm: Occurs in the part of the aorta that passes through the chest cavity.
- Cerebral (Brain) Aneurysm: Located in the arteries that supply blood to the brain. If these burst, they cause a subarachnoid hemorrhage, a specific type of stroke.
- Peripheral Aneurysms: Can occur in the arteries behind the knee (popliteal), in the groin (femoral), or in the neck (carotid).
2. Why Do They Form? (Causes and Risk Factors)
Anything that weakens the arterial walls or increases blood pressure can contribute to an aneurysm:
- Atherosclerosis: The buildup of fats and cholesterol (plaque) that hardens and weakens artery walls.
- High Blood Pressure (Hypertension): Persistent pressure against the artery walls.
- Smoking: Tobacco use significantly damages the structural integrity of blood vessels.
- Genetic Factors: Inherited conditions like Marfan Syndrome can weaken connective tissues in the heart and blood vessels.
- Age and Gender: Men over the age of 65 who have ever smoked are at the highest risk for aortic aneurysms.
3. Symptoms: The “Silent” Danger
Aneurysms are often called “silent killers” because they rarely cause symptoms until they become very large or rupture.
- If growing: You might feel a pulsating sensation (near the navel) or deep, persistent pain in the abdomen or back.
- If ruptured: Sudden, “thunderclap” headache (for brain aneurysms), extreme drop in blood pressure, rapid heart rate, and intense sharp pain.
4. Diagnosis and Treatment Strategies
Because they are often asymptomatic, many aneurysms are found “incidental” to other tests like X-rays or Ultrasounds.
Diagnosis Tools
- Ultrasound: The primary screening tool for abdominal aneurysms.
- CT Scan / MRI: Provides detailed 3D images to measure the exact size of the bulge.
- Angiogram: A specialized X-ray using dye to see the flow of blood through the artery.
Treatment Options
- “Watchful Waiting”: If the aneurysm is small, doctors monitor it every 6–12 months with imaging.
- Medication: Beta-blockers or statins to lower blood pressure and cholesterol, reducing the stress on the arterial wall.
- Endovascular Repair: A minimally invasive procedure where a stent-graft (a fabric-covered tube) is inserted into the artery to reinforce the weak spot.
- Open Surgery: The weakened section of the artery is removed and replaced with a synthetic graft.