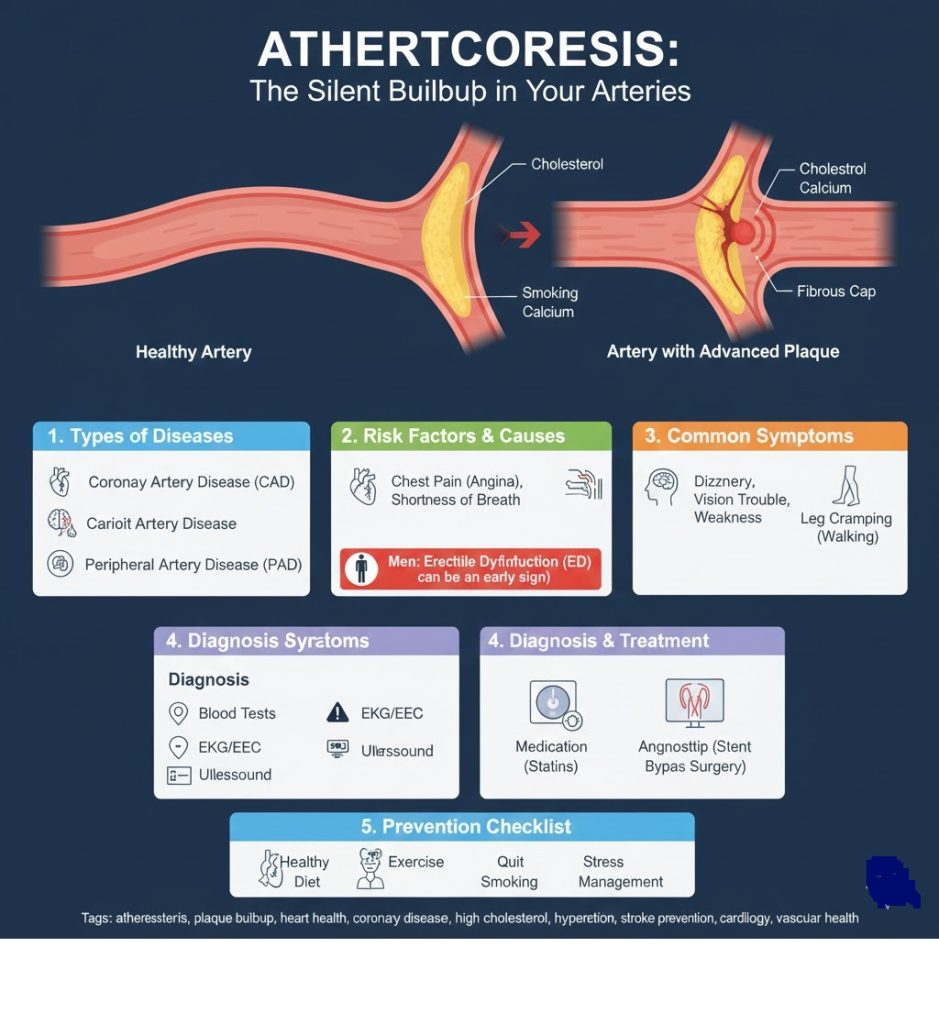
Atherosclerosis is a progressive vascular condition where “plaque”—a sticky mixture of fat, cholesterol, calcium, and blood cells—accumulates on the inner walls of your arteries. While arteriosclerosis refers generally to the hardening and thickening of arteries, atherosclerosis is the specific type caused by this plaque buildup.
Over time, this buildup narrows the pathway for blood, making the heart work harder and depriving vital organs of the oxygen they need to function.
1. Types of Diseases Caused by Atherosclerosis
Atherosclerosis is often categorized by the specific location of the blockage:
- Coronary Artery Disease (CAD): Affects the heart; can lead to chest pain (angina) or heart attack.
- Carotid Artery Disease: Affects the neck; reduces blood flow to the brain, potentially causing a stroke or TIA.
- Peripheral Artery Disease (PAD): Affects the limbs (usually legs); causes pain during movement.
- Renal Artery Stenosis: Affects the kidneys; can lead to high blood pressure or kidney failure.
- Mesenteric Artery Ischemia: Affects the intestines; leads to severe pain after eating.
2. Common Symptoms and Warning Signs
Atherosclerosis is often a “silent” condition until an artery is significantly blocked or a plaque ruptures. Symptoms depend on the location:
| Location | Key Symptoms |
| Heart | Chest pain, racing heart, shortness of breath. |
| Brain/Neck | Vision trouble, memory issues, numbness on one side of the face/body. |
| Legs | Cramping, aching, or heaviness while walking or climbing stairs. |
| Abdomen | Severe pain after meals, unintended weight loss, diarrhea. |
Note for Men: Erectile Dysfunction (ED) is often one of the earliest clinical warning signs that atherosclerosis may be developing elsewhere in the body.
3. Risk Factors and Causes
While the exact trigger is unknown, damage to the inner lining of the artery allows plaque to start forming—often as early as childhood.
- Medical Conditions: High blood pressure, high cholesterol, diabetes, and inflammatory diseases (like RA or psoriasis).
- Lifestyle: Smoking/tobacco use, a diet high in saturated fats, and physical inactivity.
- Biology: Risk increases significantly for men over 45 and women over 55.
4. Diagnosis and Treatment
To diagnose the condition, healthcare providers use a combination of physical exams (listening for a “bruit” or whooshing sound in the arteries) and specialized tests:
- Blood Tests: To check cholesterol and sugar levels.
- EKG/ECG: To check heart rhythm.
- Ultrasound: To visualize blood flow and plaque in the neck or limbs.
- Angiography: Using dye and X-rays to see inside the arteries.
Treatment Pathways
- Lifestyle Changes: Focusing on a heart-healthy diet, regular exercise, and stress management.
- Medications: Statins for cholesterol, blood pressure medicine, or anti-platelet drugs to prevent clots.
- Procedures: Angioplasty (inflating a balloon to widen the artery) or Bypass Surgery (creating a new path for blood flow).
5. Prevention Checklist
- Diet: Prioritize whole grains, fruits, and vegetables.
- Activity: Aim for regular, moderate exercise.
- Sleep: Ensure 7–9 hours of quality sleep.
- Habits: Quit smoking and limit alcohol intake.