An ischemic stroke occurs when the blood supply to a part of the brain is suddenly interrupted. Since blood carries essential oxygen and nutrients, brain cells begin to die within minutes of being deprived. This makes a stroke a medical emergency where “time is brain.”
1. Types of Ischemic Stroke Causes
Ischemic strokes account for about 87% of all stroke cases. They are primarily caused by blockages in two ways:
- Thrombotic Stroke: A blood clot (thrombus) forms directly inside one of the arteries supplying blood to the brain. This is often caused by atherosclerosis (plaque buildup).
- Embolic Stroke: A blood clot or plaque fragment forms elsewhere in the body—frequently the heart or the large arteries of the upper chest and neck—and travels through the bloodstream to lodge in a narrower brain artery.
- Atrial Fibrillation (AFib): An irregular heart rhythm can cause blood to pool in the heart, forming clots that are easily swept toward the brain.
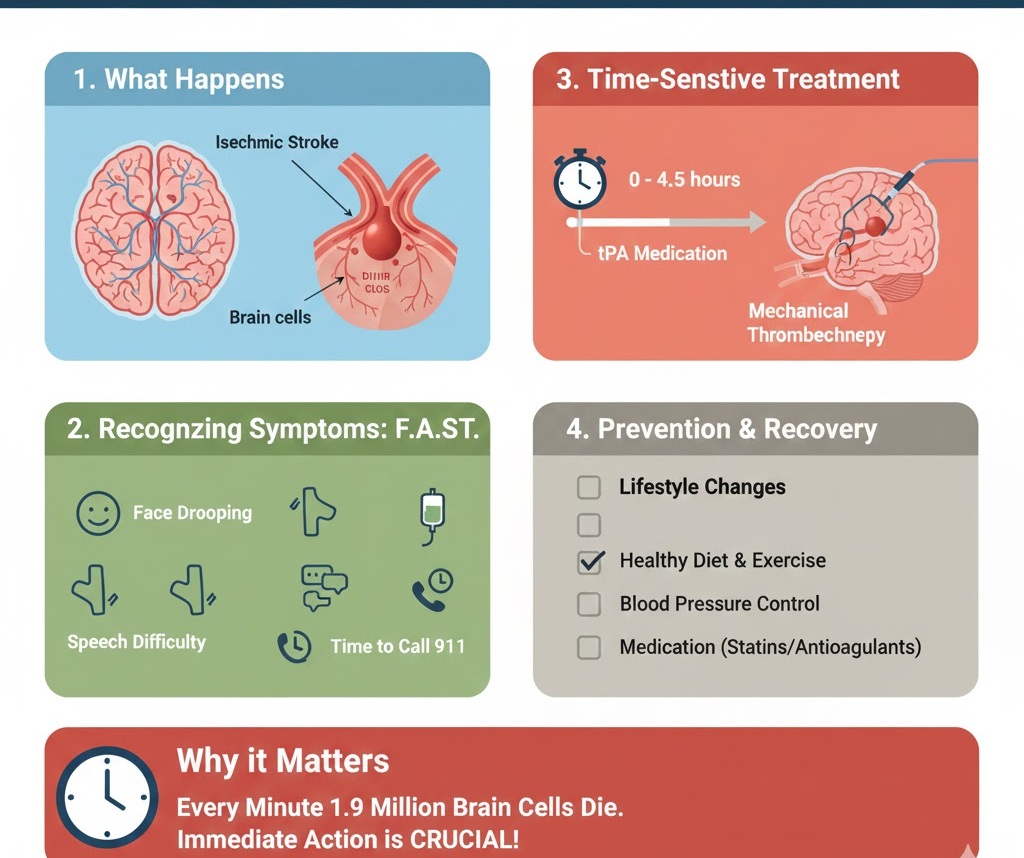
2. Recognizing Symptoms: The F.A.S.T. Method
Stroke symptoms usually appear without warning. Use the F.A.S.T. acronym to identify a stroke and take action:
- F — Face: Ask the person to smile. Does one side of the face droop?
- A — Arms: Ask the person to raise both arms. Does one arm drift downward?
- S — Speech: Ask the person to repeat a simple phrase. Is their speech slurred or strange?
- T — Time: If you observe any of these signs, call 911 immediately.
3. Diagnosis and Time-Sensitive Treatment
Doctors use physical exams, blood tests, and imaging like CT scans or MRIs to confirm the stroke is ischemic (caused by a clot) and not hemorrhagic (caused by bleeding).
Emergency Treatments
- tPA (Thrombolytics): Often called “clot-busters,” these medicines can dissolve the clot and restore blood flow. They must be administered within a few hours of the first symptoms.
- Mechanical Thrombectomy: A procedure where a surgeon threads a catheter into the brain to physically grab and remove the clot.
4. Prevention and Recovery
After the emergency has passed, the focus shifts to rehabilitation (physical, occupational, or speech therapy) and preventing a second stroke.
| Risk Factor | How to Manage It |
| High Blood Pressure | The #1 risk factor; managed with diet and medication. |
| Cholesterol | Managed through statins and reducing saturated fats. |
| Diabetes | Keeping blood sugar within a target range to protect blood vessels. |
| Atrial Fibrillation | Using blood thinners (anticoagulants) to prevent heart-based clots. |