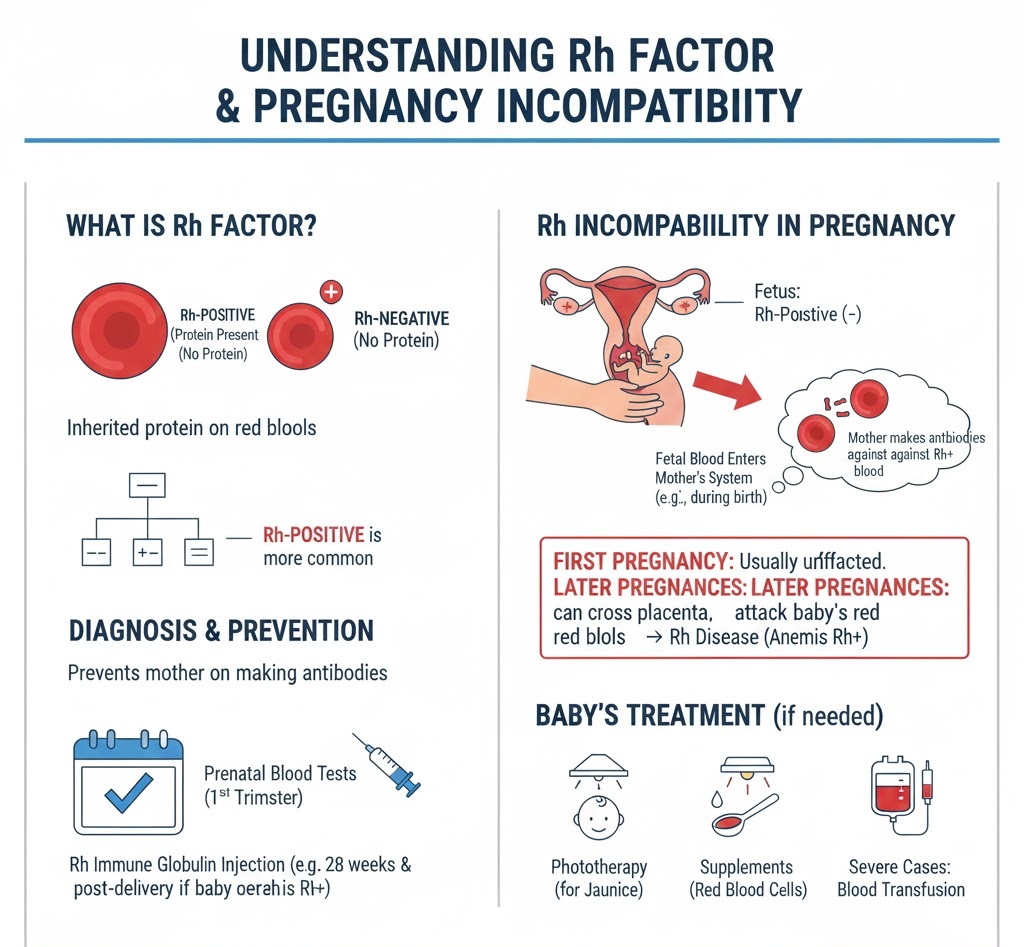
The Rh factor is a specific protein found on the surface of red blood cells. Just like your blood type (A, B, AB, or O), the Rh factor is inherited from your parents.
- Rh-positive (+): You have the protein on your blood cells. (Most people fall into this category).
- Rh-negative (-): You do not have the protein.
While being Rh-negative does not impact your personal health, it becomes a critical factor to monitor during pregnancy.
What is Rh Incompatibility?
Rh incompatibility occurs when a pregnant person is Rh-negative but the fetus is Rh-positive.
If the fetus’s blood enters the mother’s bloodstream (which often happens during birth, miscarriage, or abdominal trauma), the mother’s immune system identifies the Rh protein as a “foreign invader.” This triggers the production of antibodies designed to attack Rh-positive blood cells.
Note on Future Pregnancies: Usually, the first pregnancy is not affected because the body doesn’t produce enough antibodies quickly enough. However, once those antibodies exist, they stay in the body. In a subsequent pregnancy with an Rh-positive fetus, these antibodies can cross the placenta and attack the baby’s red blood cells, leading to severe anemia or Rh disease.
Diagnosis and Treatment
Detection is simple and begins at the very first prenatal visit:
- Blood Tests: Providers check your blood type and Rh factor, as well as an “antibody screen” to see if your body has already started producing Rh antibodies.
Prevention and Management:
If you are Rh-negative, the standard treatment is highly effective at preventing complications:
- Rh Immune Globulin Injection: This medicine (often called RhoGAM) is typically given around week 28 of pregnancy and again within 72 hours after delivery if the baby is confirmed to be Rh-positive. It stops your immune system from “seeing” the Rh-positive cells and forming antibodies.
- Infant Treatment: If a baby is born with Rh disease, they may receive phototherapy for jaundice, supplements, or in rare, severe cases, a blood transfusion.