Insomnia is a prevalent sleep disorder characterized by persistent difficulties in falling asleep, staying asleep, or experiencing non-restorative sleep. Even with the opportunity for a full night’s rest, individuals with insomnia often wake up feeling unrefreshed, leading to significant daytime impairment.
Types of Insomnia
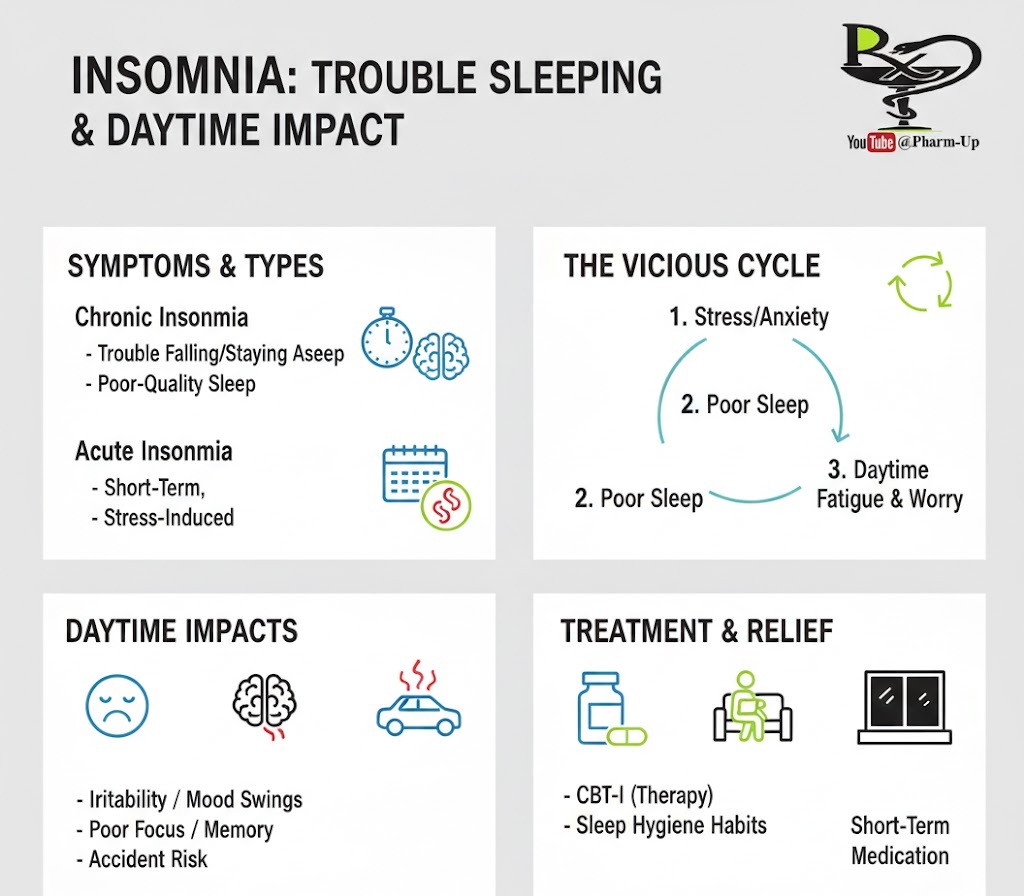
Understanding the duration and cause of your sleeplessness is the first step toward treatment:
- Acute Insomnia: Short-term episodes lasting a few days or weeks. This is usually triggered by life events like work stress, exams, family pressures, or travel.
- Chronic Insomnia: Occurs at least three nights a week and lasts for one month or longer.
- Secondary Insomnia: The most common form of chronic insomnia. It is a symptom of another issue, such as depression, chronic pain, asthma, or the use of substances like caffeine and alcohol.
- Primary Insomnia: Sleeplessness that is not directly associated with any other health condition.
Risks and Vulnerabilities
While anyone can experience insomnia, certain groups and factors carry a higher risk:
- Gender and Age: It occurs more frequently in women and older adults.
- Lifestyle: High-stress levels, inactive lifestyles, and shift work (night shifts) significantly disrupt the body’s internal clock.
- Socioeconomic Factors: Research suggests that lower income levels and chronic emotional distress (like divorce) are linked to higher insomnia rates.
Symptoms and Daytime Impact
Insomnia isn’t just about what happens at night; it affects your entire day. Common signs include:
- Lying awake for long periods before finally drifting off.
- Waking up frequently during the night or waking up much earlier than intended.
- Daytime Consequences: Irritability, anxiety, and “brain fog” (difficulty focusing or remembering).
- Safety Risks: Severe drowsiness increases the risk of errors at work and dangerous motor vehicle accidents.
Diagnostic Approach and Treatment
Doctors typically diagnose insomnia through a Sleep History (tracking habits over 1-2 weeks) and physical exams to rule out underlying illnesses. In complex cases, a Sleep Study (polysomnography) may be ordered.
Management Strategies:
- Cognitive Behavioral Therapy for Insomnia (CBT-I): Often recommended as the first-line treatment for chronic insomnia. It helps patients change thoughts and behaviors that prevent sleep.
- Sleep Hygiene: Establishing a consistent wake-up time, avoiding afternoon caffeine, and making the bedroom a “tech-free” zone.
- Medications: Doctors may prescribe sleep aids for short-term use to help re-establish a healthy rhythm.
- Addressing Underlying Issues: Treating the primary cause (like sleep apnea or anxiety) often resolves the secondary insomnia.