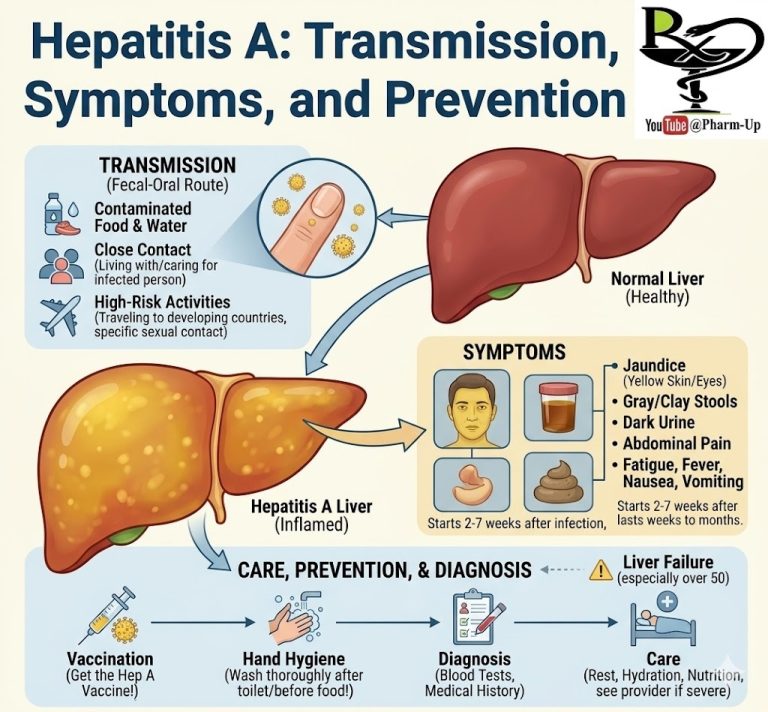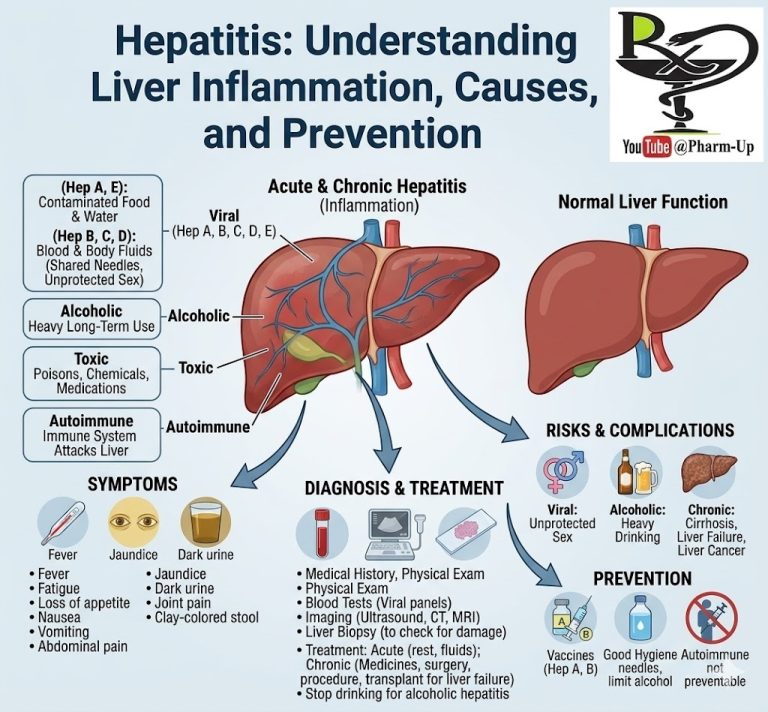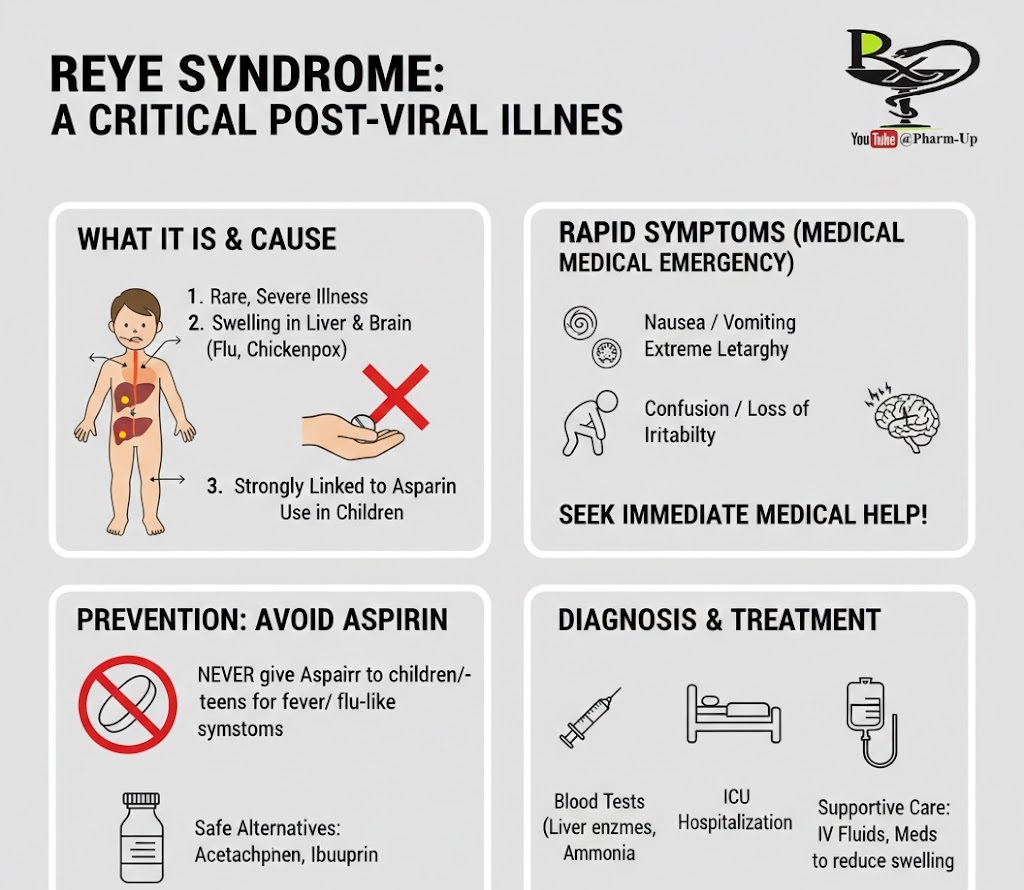
Reye (pronounced “rise”) syndrome is a rare but life-threatening condition that causes swelling in the liver and brain. It almost always occurs as a child or teenager is recovering from a viral infection, most commonly the flu (influenza) or chickenpox. While the exact cause is unknown, it is highly associated with the use of aspirin during these viral illnesses.
How Reye Syndrome Develops
Reye syndrome typically develops 3 to 5 days after the onset of a viral infection. It begins with a sudden drop in blood sugar (hypoglycemia) and a rise in ammonia and acidity in the blood. Simultaneously, the liver may swell and develop fatty deposits, while the brain may swell (cerebral edema), leading to neurological symptoms.
Symptoms to Watch For
Because Reye syndrome can progress rapidly to a medical emergency, early recognition is vital. Symptoms usually appear in stages:
- Initial Signs: Persistent or projectile vomiting and unusual sleepiness or lethargy (listlessness).
- Behavioral Changes: Irritability, aggressiveness, confusion, or irrational behavior.
- Advanced Signs: Delirium, seizures (convulsions), and loss of consciousness.
Warning: If these symptoms appear during or shortly after a viral illness, seek emergency medical care immediately. Rapid treatment is the only way to prevent permanent brain damage or death.
The Aspirin Connection
Extensive research has linked the use of aspirin (salicylates) during viral infections to the development of Reye syndrome.
- The Recommendation: Health care professionals strongly advise against giving aspirin to children or teenagers unless specifically directed by a doctor for a chronic condition (like Kawasaki disease).
- Safe Alternatives: Use acetaminophen (Tylenol) or ibuprofen (Advil/Motrin) to manage fever or pain in young patients.
- Check Labels: Be aware that “hidden” aspirin can be found in products like Pepto-Bismol and some cold medications (listed as salicylates, acetylsalicylic acid, or salicylic acid).
Diagnosis and Management
There is no specific cure for Reye syndrome; treatment is supportive and focuses on protecting the organs while the body recovers.
- Diagnosis: Doctors may use blood tests (to check liver function and ammonia levels), a spinal tap (to rule out meningitis), or a liver biopsy.
- Hospitalization: Treatment always occurs in an intensive care unit (ICU).
- Interventions: Intravenous (IV) fluids with glucose to restore blood sugar, diuretics to reduce brain swelling, and medications to lower ammonia levels.