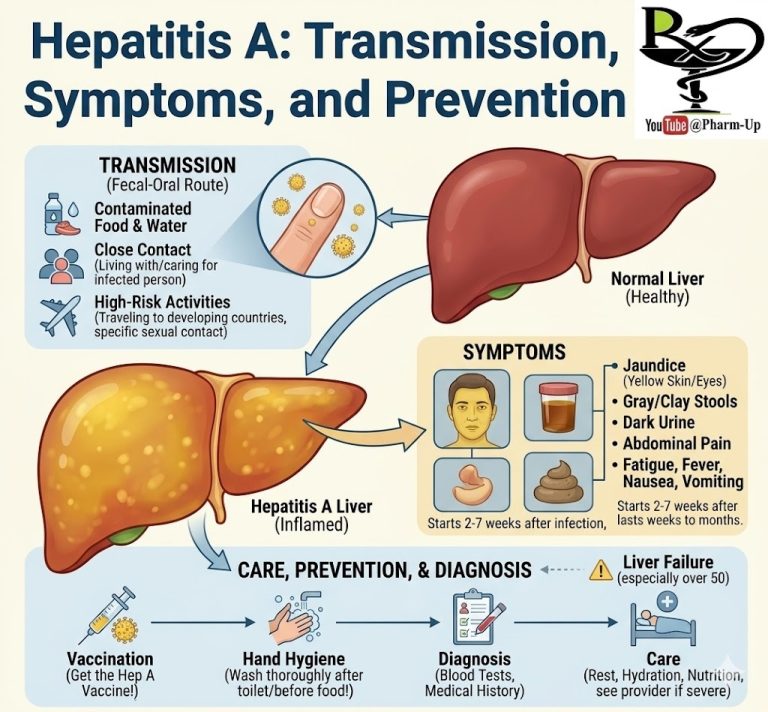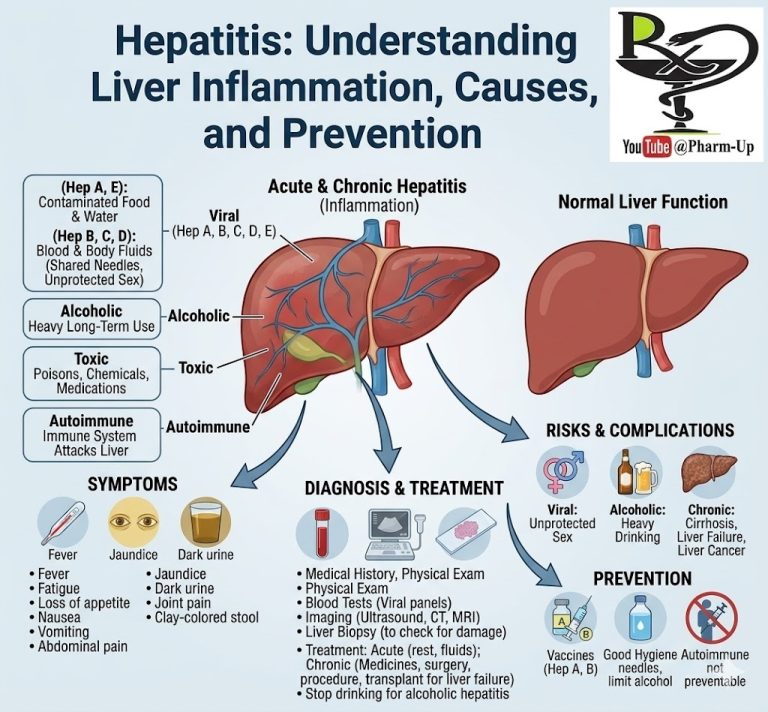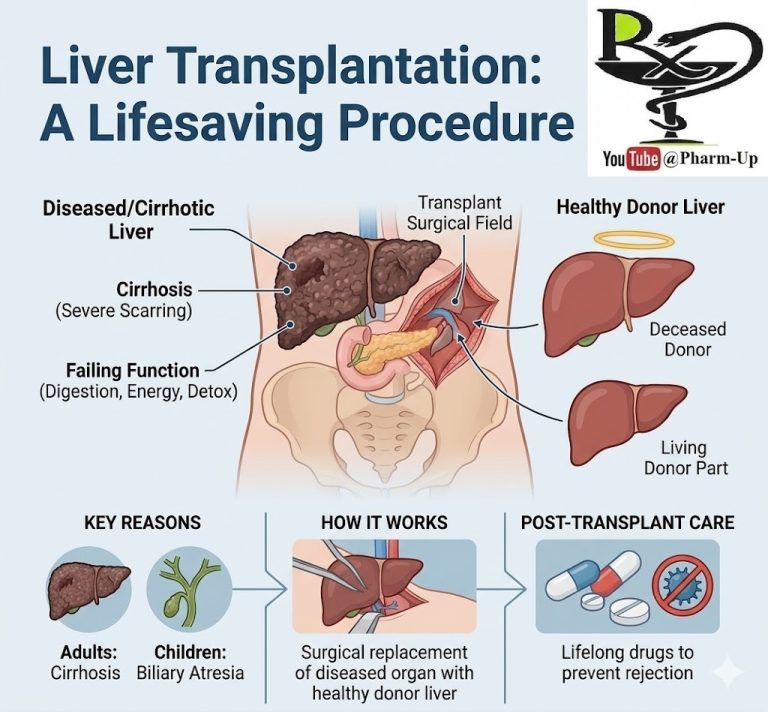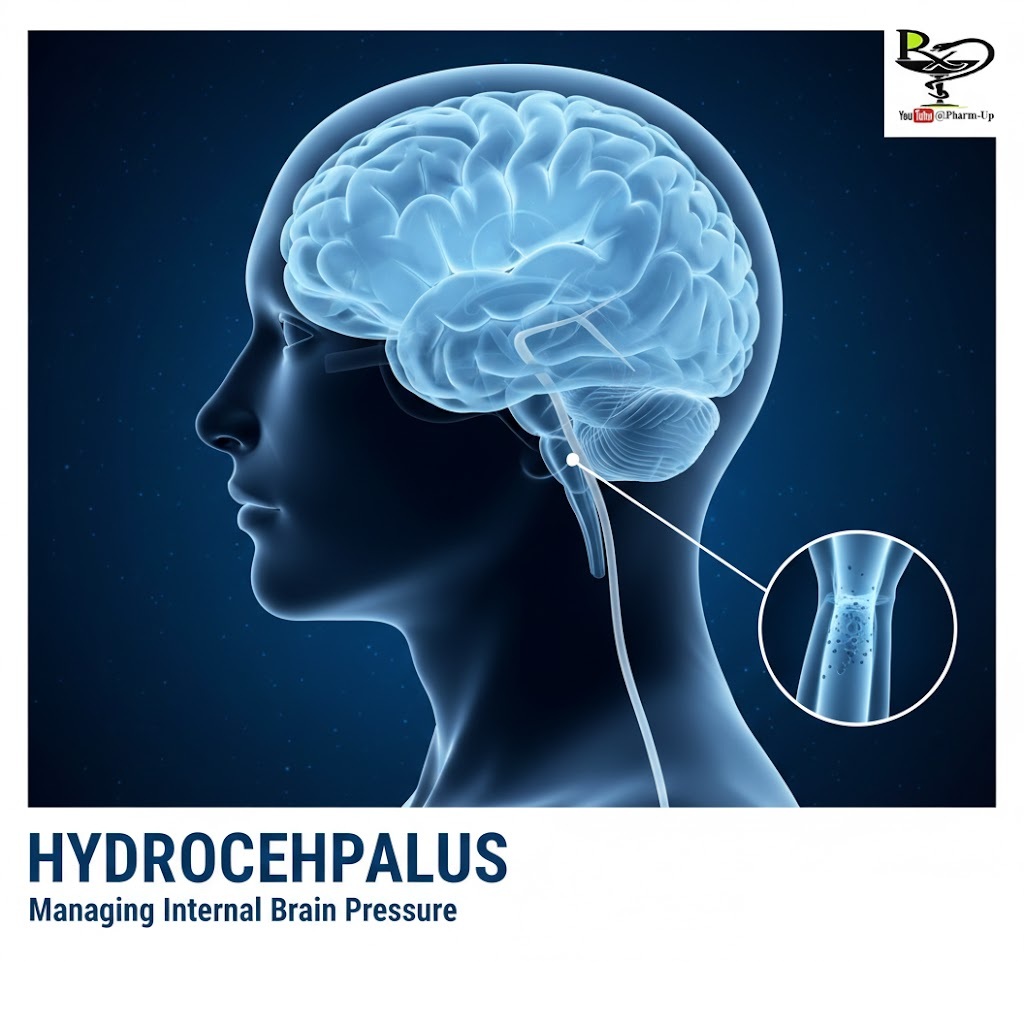
Hydrocephalus, often colloquially referred to as “water on the brain,” is a condition characterized by an abnormal accumulation of Cerebrospinal Fluid (CSF) within the ventricles (cavities) of the brain. While CSF is vital for cushioning the brain and clearing waste, too much of it creates a dangerous “tight fit” inside the skull.
The Role of Cerebrospinal Fluid (CSF)
Normally, CSF flows through the ventricles, bathes the brain and spinal cord, and is then absorbed into the bloodstream. In hydrocephalus, this flow is disrupted like a clogged plumbing system, leading to increased intracranial pressure.
Congenital vs. Acquired
The condition is categorized based on when it develops:
- Congenital (At Birth): Resulting from complex environmental or genetic factors during fetal development. In infants, because the skull bones haven’t fused yet, the most visible sign is a rapidly enlarging head or a bulging “soft spot” (fontanel).
- Acquired (Any Age): This can be triggered by external factors such as:
- Severe head trauma or brain bleeds.
- Infections like meningitis.
- Brain tumors that physically block the fluid’s path.
Recognizing the Symptoms
Because the brain is being compressed, symptoms affect both physical and cognitive functions:
- Physical: Chronic headaches, nausea, blurred or double vision, and loss of bladder control.
- Cognitive: Sudden “brain fog,” memory loss, or changes in personality.
- Movement: A distinctive “shuffling” gait or general balance instability.
Surgical Intervention: The Shunt System
The most common and effective treatment for hydrocephalus is the surgical implantation of a shunt.
- The Valve: A pressure-activated valve is placed near the brain.
- The Tube: A flexible catheter runs under the skin from the brain to another part of the body (usually the abdomen or a heart chamber).
- The Drainage: The excess CSF is diverted to these areas, where it is harmlessly reabsorbed into the body.
Life After Diagnosis
While hydrocephalus is life-threatening if left untreated, modern neurosurgery allows many patients to lead full, active lives. Ongoing monitoring is essential, as shunts may occasionally require “revisions” or adjustments over time.