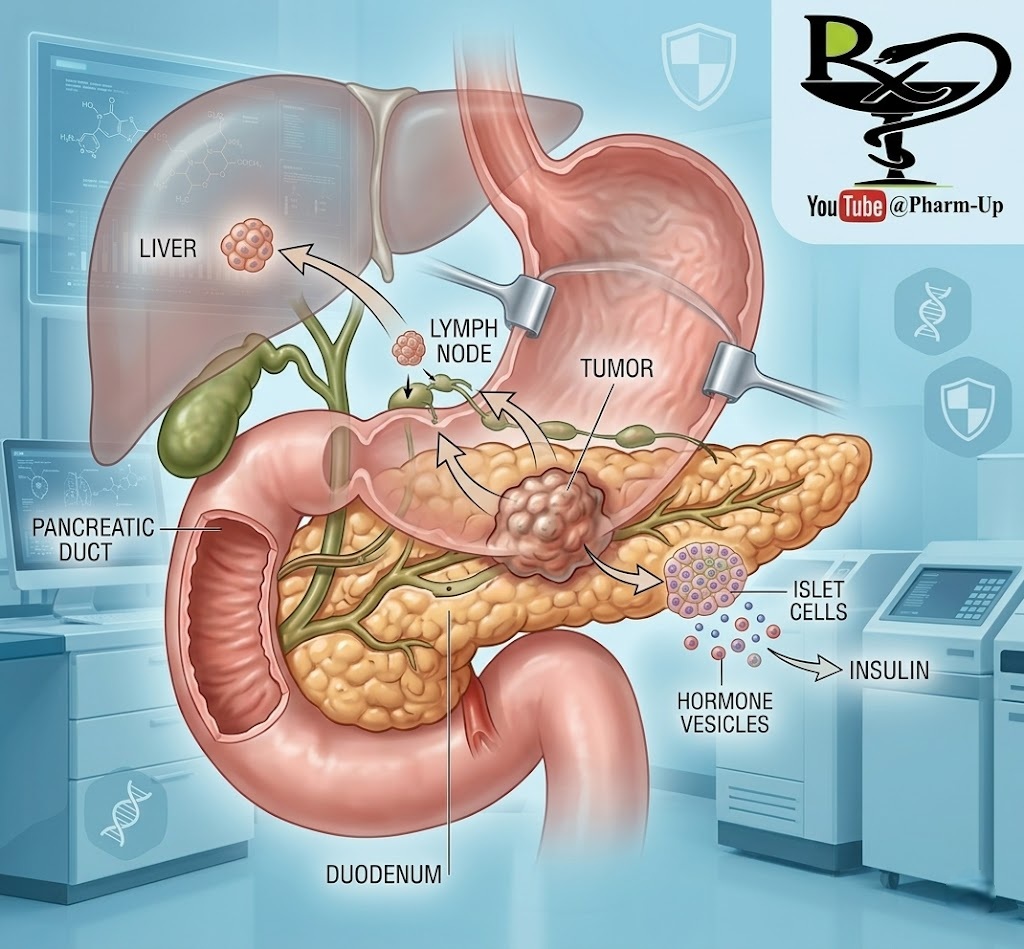
The pancreas is a critical gland situated deep within the abdomen, responsible for secreting digestive enzymes and regulating blood sugar through hormone production. Pancreatic cancer primarily originates in the enzyme-producing cells and is known for its aggressive nature and the difficulty of early diagnosis.
Major Risk Factors
Understanding the contributors to pancreatic health is the first step in prevention. Key risk factors include:
- Lifestyle Habits: Smoking is one of the most significant preventable risks.
- Chronic Conditions: Long-term diabetes and chronic pancreatitis (persistent inflammation).
- Genetic Predisposition: Certain inherited syndromes passed down through families.
The “Silent” Symptoms
Pancreatic cancer is notoriously difficult to catch early because the organ is tucked behind other structures, making tumors impossible to feel during a routine check-up. Symptoms are often vague until the disease reaches an advanced stage:
- Jaundice: Yellowing of the skin and eyes occurs if the tumor blocks the bile duct.
- Localized Pain: Persistent discomfort in the upper abdomen that may radiate to the back.
- Unexplained Changes: Rapid weight loss and unusual fatigue.
Diagnostic Procedures
Since routine physicals rarely uncover pancreatic tumors, doctors utilize a multi-step approach for diagnosis:
- Imaging Tests: CT scans, MRIs, and ultrasounds to visualize the hidden gland.
- Laboratory Work: Specific blood tests to look for tumor markers.
- Biopsy: Extracting a tissue sample to confirm the presence and type of cancer cells.
Current Treatment Landscapes
Because this cancer spreads quickly, medical teams often combine several treatment modalities:
- Conventional Methods: Surgery to remove the tumor, along with radiation and chemotherapy.
- Targeted Therapy: A modern approach using drugs designed to identify and attack specific cancer cells. This method aims to be more effective while causing less collateral damage to healthy cells.