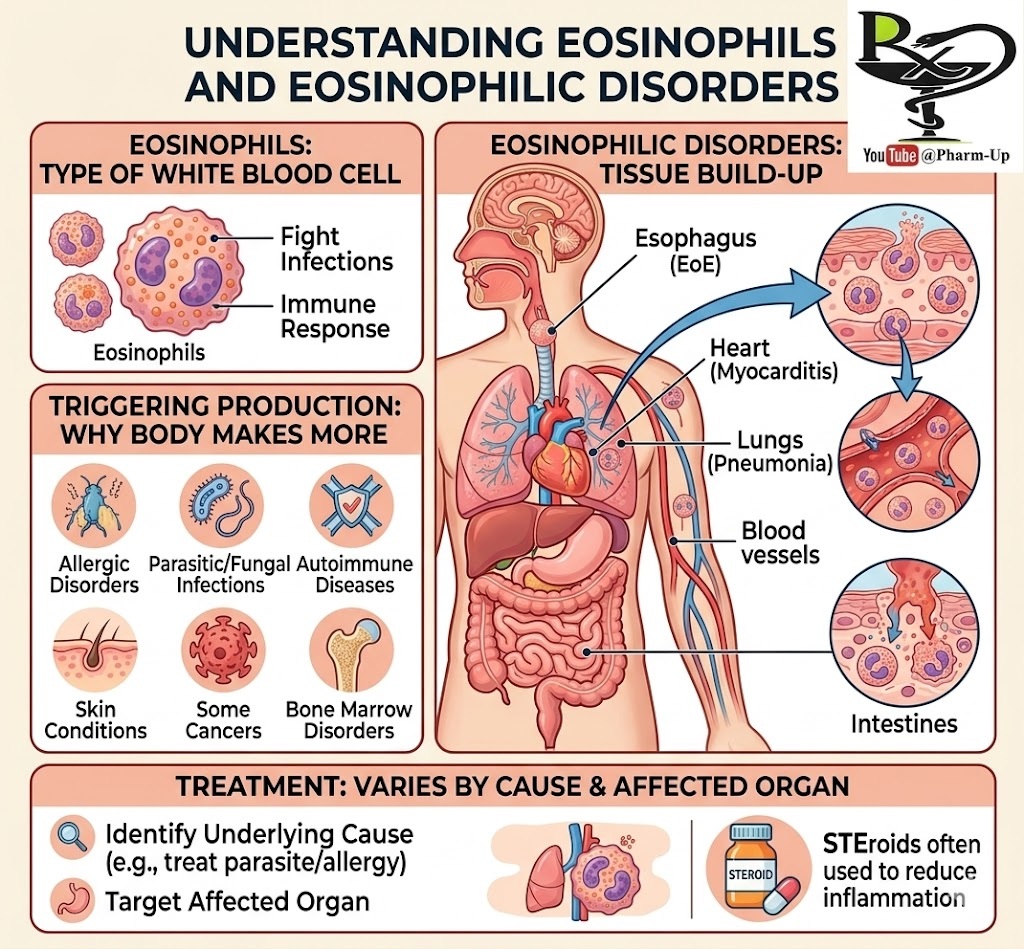
Eosinophils are a critical type of white blood cell. Their primary functions are to help the body fight off infections and modulate the immune response. When they function correctly, they are a protective force. However, in certain conditions, they can accumulate excessively, leading to significant inflammation and tissue damage.
The Normal Level and Triggers for Production
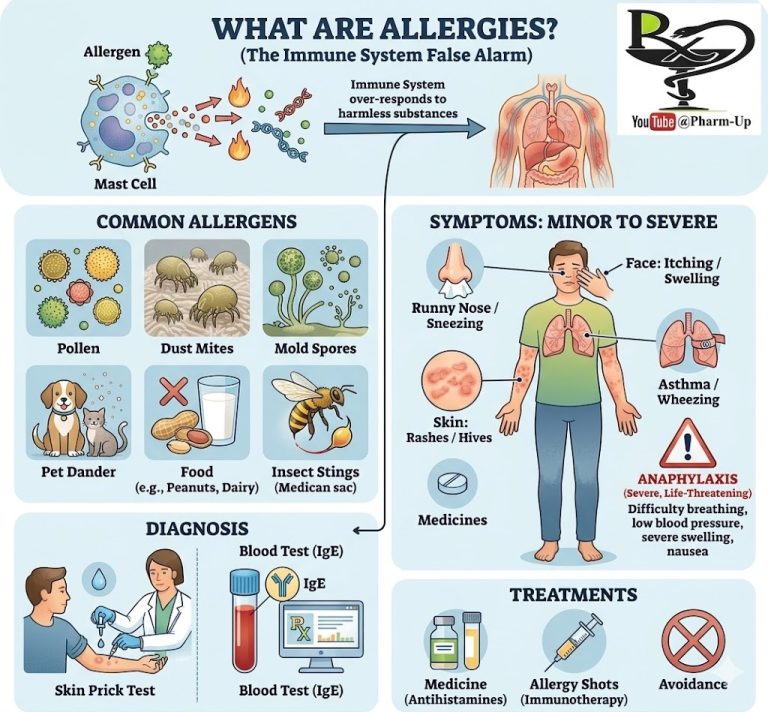
Under typical circumstances, the blood contains only a small number of eosinophils. However, the body is triggered to produce more in response to several specific signals. Common causes for an elevated eosinophil count (known as eosinophilia) include:
- Allergic disorders
- Skin conditions
- Parasitic and fungal infections
- Autoimmune diseases
- Some cancers
- Bone marrow disorders
Eosinophilic Disorders: Tissue Infiltration
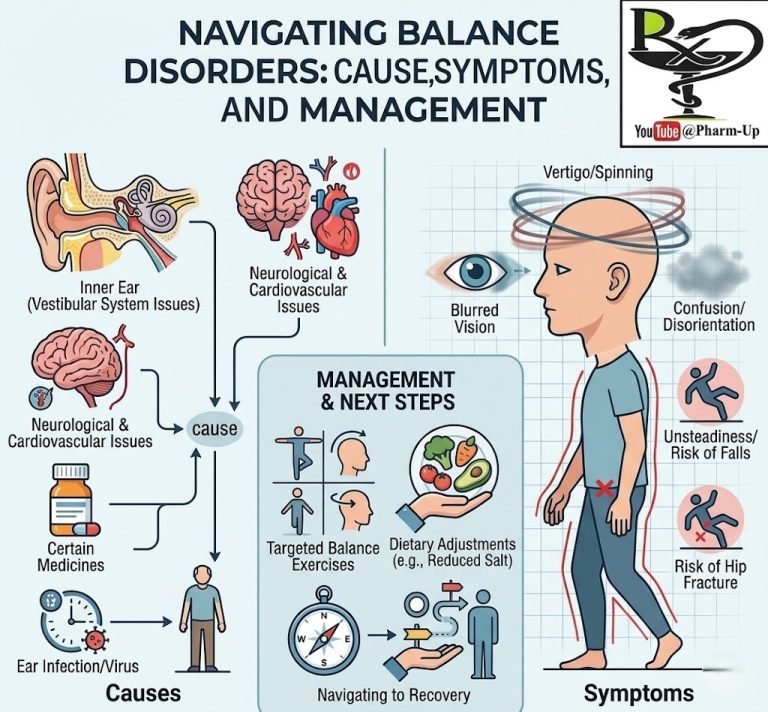
In certain disorders, these cells don’t just increase in number; they migrate from the bloodstream into surrounding organs and tissues, where they build up and release inflammatory chemicals. This infiltration can affect many parts of the body, including the esophagus, heart, lungs, blood, and intestines.
A common example of tissue-specific infiltration is eosinophilic esophagitis (EoE), where eosinophils build up in the esophagus, often in response to food or environmental allergens, causing inflammation and difficulty swallowing.
Diagnosis and Treatment
Diagnosing an eosinophilic disorder typically requires a combination of complete blood counts, medical history, and, most importantly, tissue biopsies from the affected organ to directly observe and count the infiltrating cells.
Treatment approaches are highly specialized and depend heavily on:
- The specific underlying cause (e.g., treating a parasite vs. an allergy).
- Which specific part of the body is affected.
In many cases, regardless of the target organ, corticosteroids (often just called “steroids”) are a primary component of treatment to reduce the intense inflammation.